March SonoProps
Welcome to our March SonoProps! Forget winter, here comes spring…
Our first SonoProps for this month goes to Dr. Jaspreet Kaur.
She was scanning a 67-year-old male with a history of hypertension, hyperlipidemia, aortic aneurysm status post mechanical aortic valve replacement on warfarin, and a left inguinal hernia presented to the Emergency Department with abdominal pain. The patient stated that two days prior to presentation, he noticed an area of point tenderness along the left lateral abdominal wall. The pain was worse with bearing down, direct palpation and flexing his trunk
He denied prior similar symptoms. The patient denied fever, chills, nausea, vomiting, diarrhea, constipation, chest pain, or shortness of breath. He denied any trauma or injuries.
Given the patient’s focal abdominal wall tenderness, a POCUS exam of the left lower quadrant at the point of maximal pain was performed.
She obtained the following images:
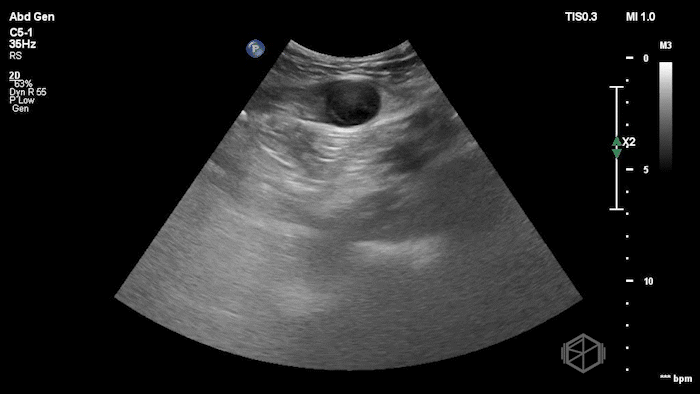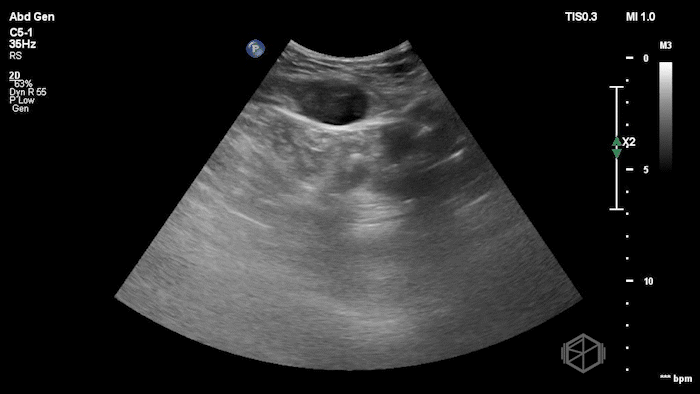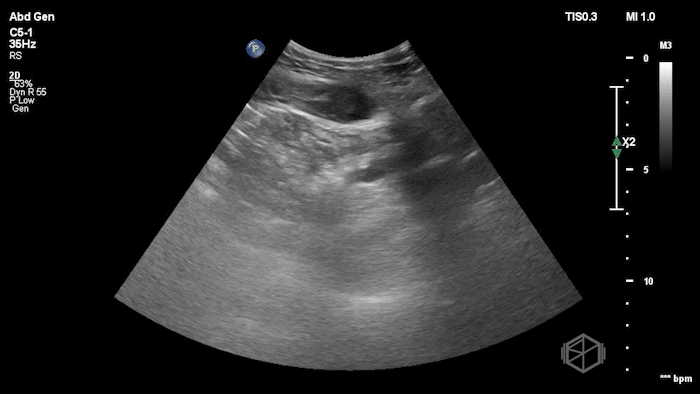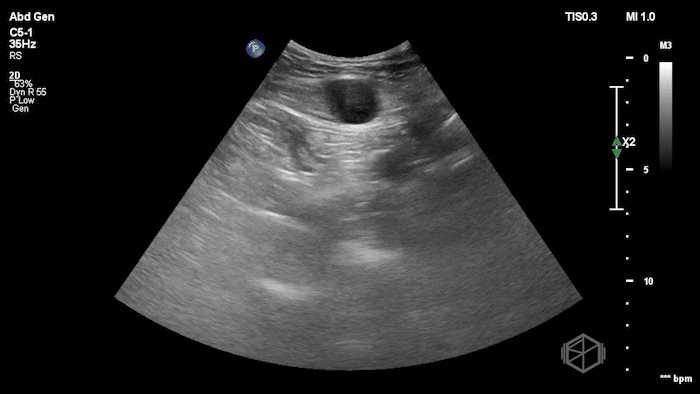
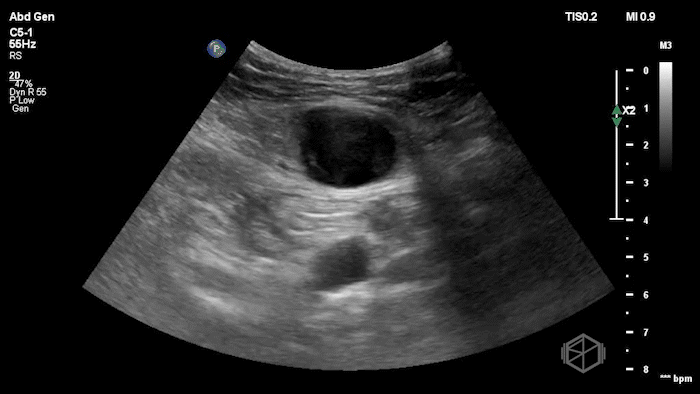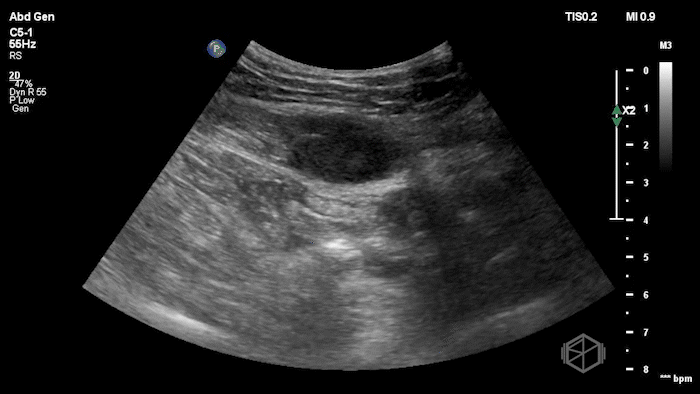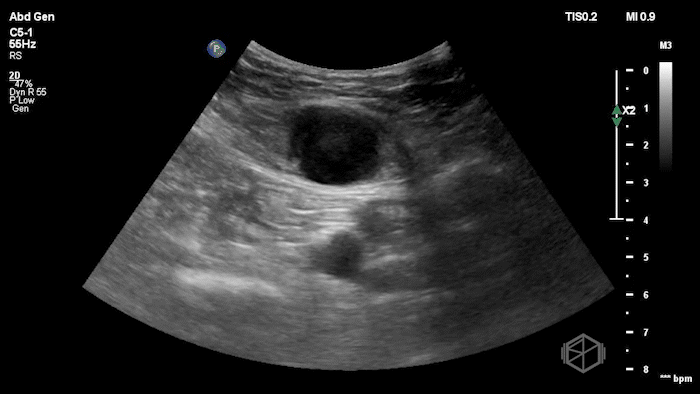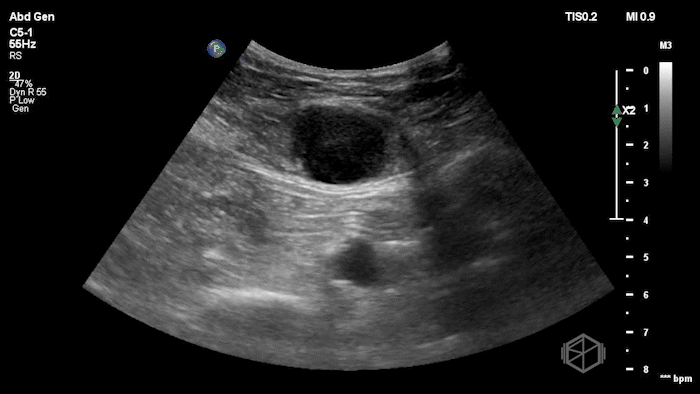
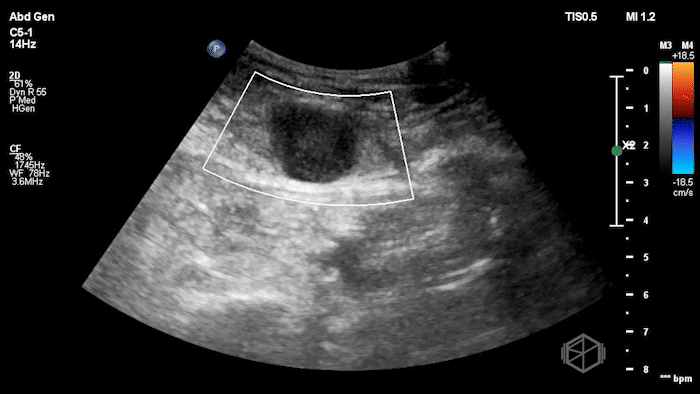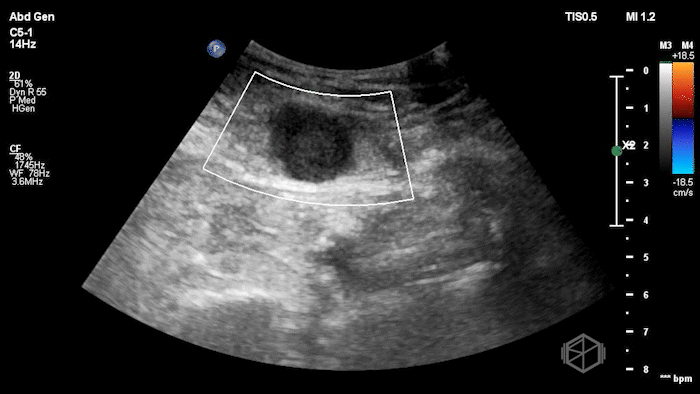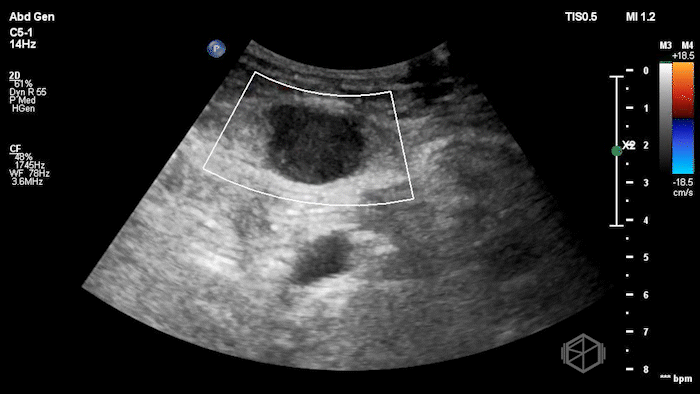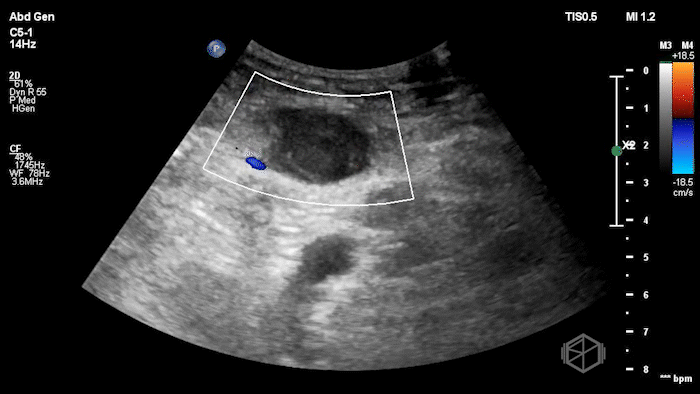
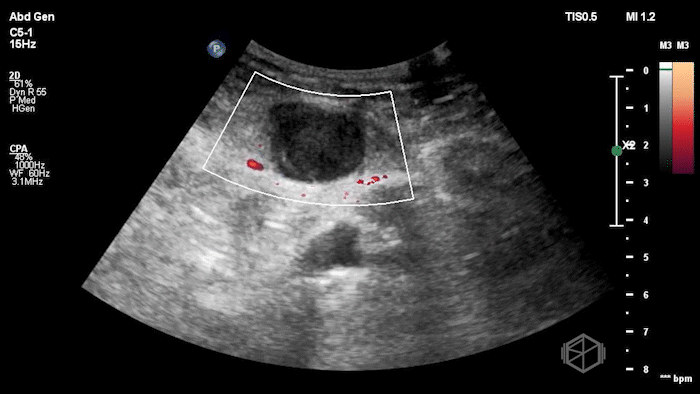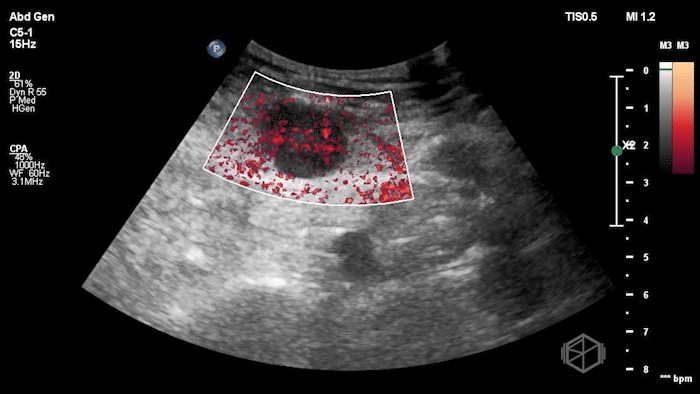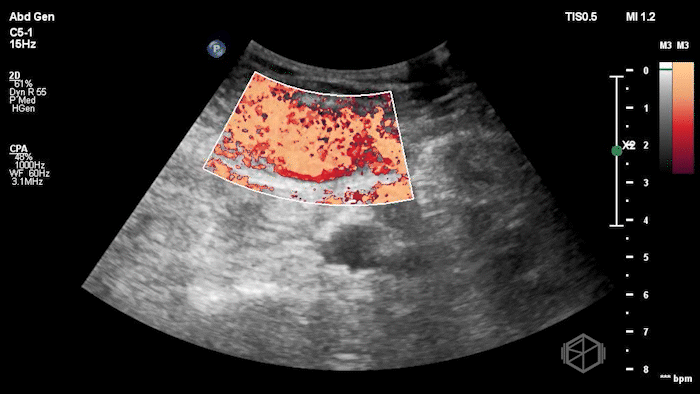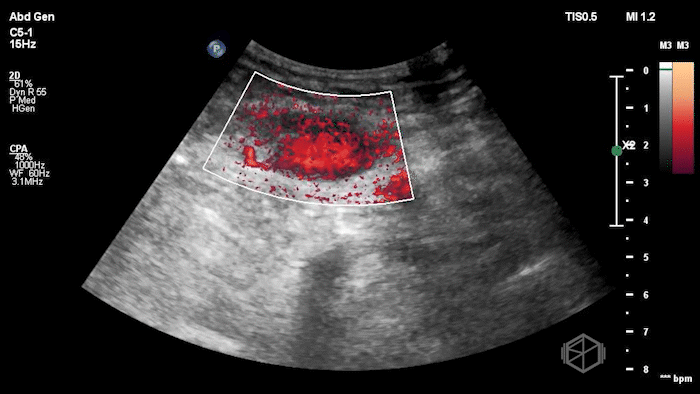
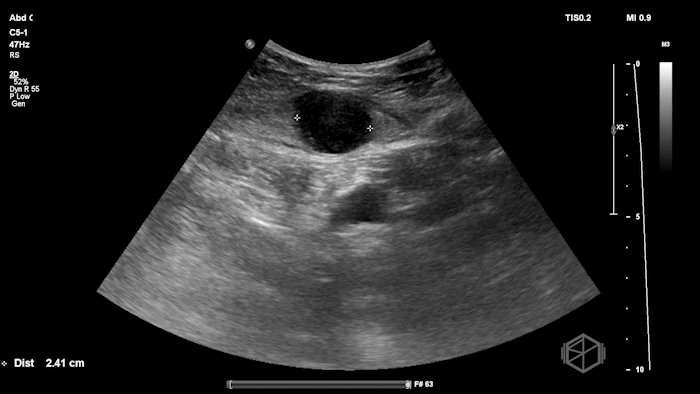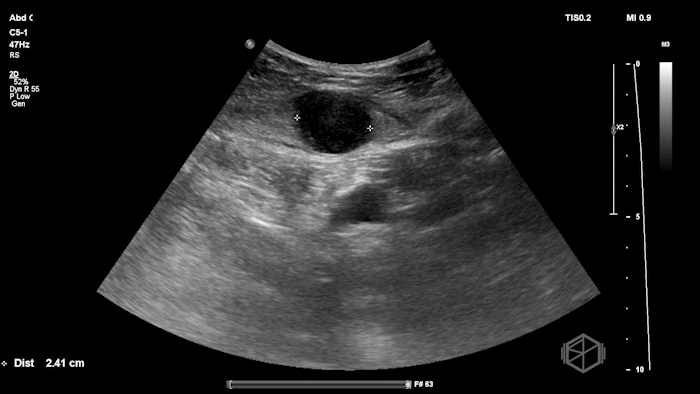
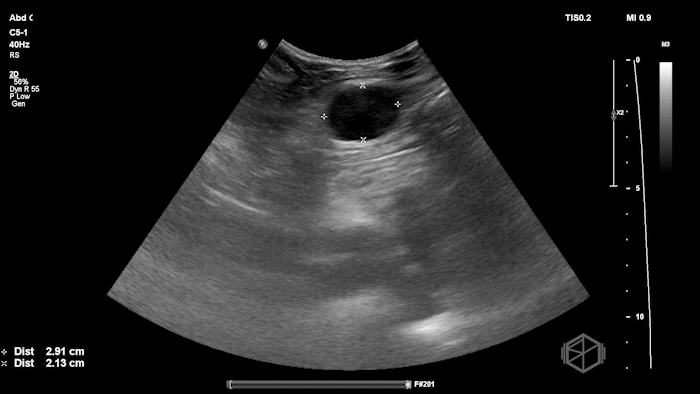
The POCUS shows an hypoechoic circular mass within the rectus muscle. There is no active color doppler flow suggesting likely no active bleeding.
Diagnosis: Rectus sheath hematoma (RSH)
Learning Points:
RSH is an uncommon but important cause of abdominal pain.
It occurs due to bleeding into the rectus muscle sheath, most commonly from injury to the superior or inferior epigastric vessels or from direct muscle tear. It can mimic intra-abdominal pathology such as appendicitis, diverticulitis, or hernia. (📚 PMID: 10556453, 6235761, 145260)
Below the arcuate line (~5 cm below the umbilicus) the posterior rectus sheath is absent, leaving the epigastric vessels protected only by transversalis fascia. Increased abdominal pressure or muscle contraction can therefore more easily injure these vessels. RSH typically remains unilateral and rarely crosses the midline due to the linea alba. (📚 PMID: 23791004)
Anticoagulation is one of the most significant risk factors.
Anticoagulation, coughing, trauma, hypertension, and abdominal strain are all associated with development of RSH. As anticoagulant use has increased, the incidence of RSH has also risen. (📚 PMID: 10556453)
Abdominal wall pathology should be suspected when pain is focal and reproducible with abdominal tensing.
A positive Carnett’s sign (accentuated localized tenderness with abdominal wall tensing) supports abdominal wall pain rather than visceral pathology. (📚 PMID: 12003414)
POCUS can rapidly identify RSH.
POCUS is useful for rapid diagnosis, but CT remains the gold standard.
Ultrasound has a sensitivity of approximately 80–90% for RSH, but CT approaches 98% sensitivity and specificity and allows classification using the Berna system (Types I–III), which correlates with severity and need for intervention. (📚 PMID: 23791004)
Management is typically conservative.
Our next SonoProps goes to Dr. Gena Koutsounadis.
A 94-year-old female with a history of dementia presented with tachycardia and hypotension.
POCUS cardiac evaluation was performed and demonstrated normal cardiac activity without right ventricular dilation. A small known pericardial effusion was visualized without evidence of tamponade physiology.
Given persistent tachycardia and hypotension, further POCUS evaluation was performed.
A lower extremity DVT ultrasound performed by Dr. Koutsounadis demonstrated the following:
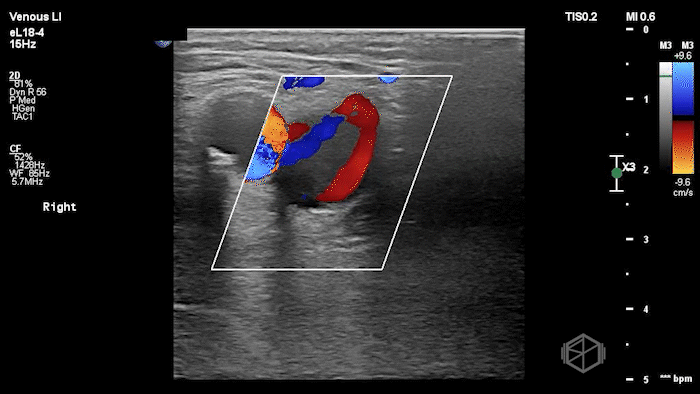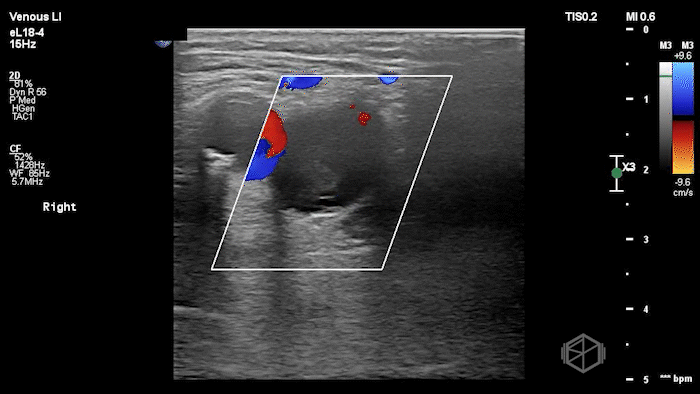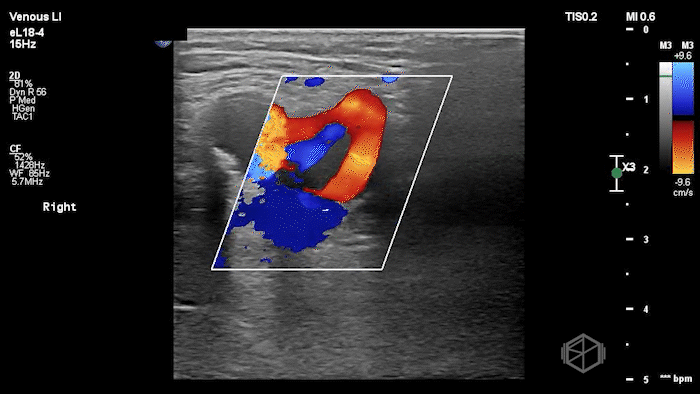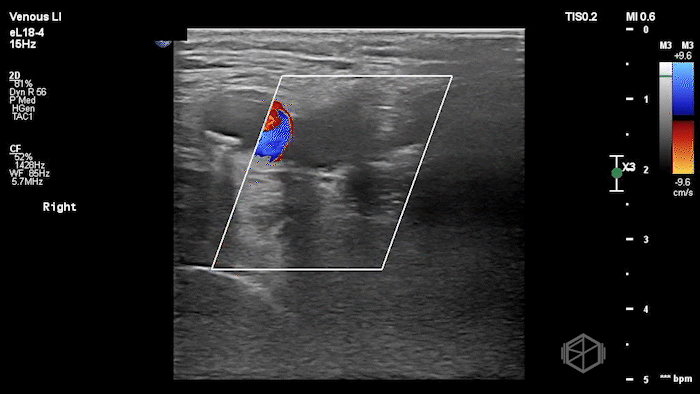
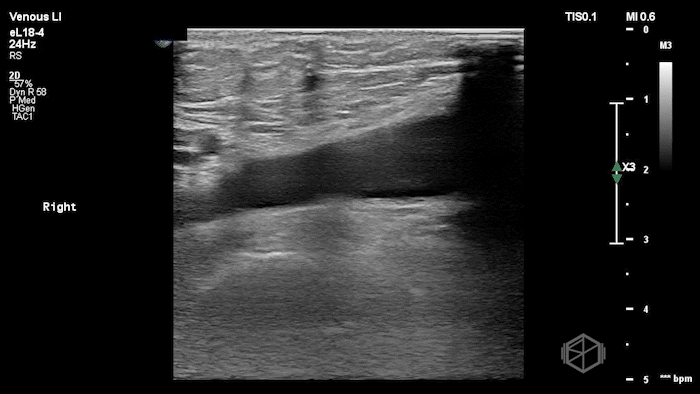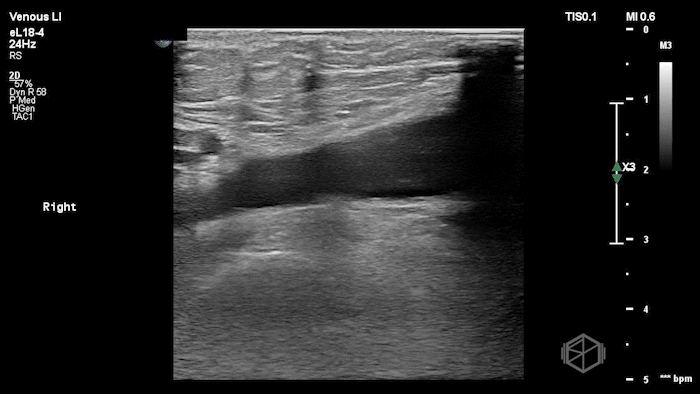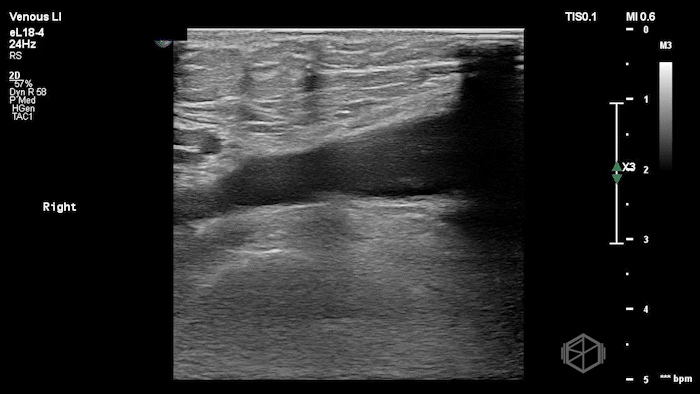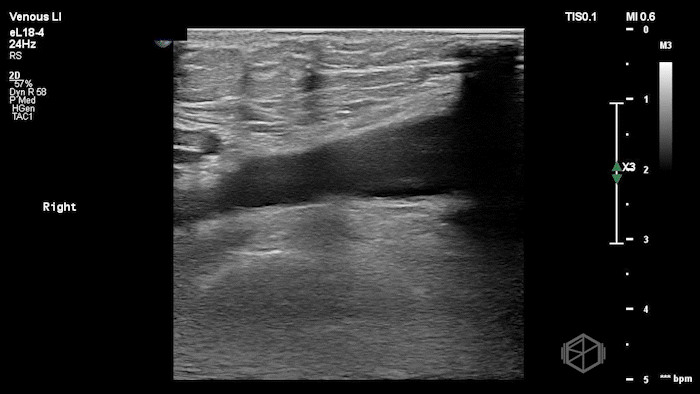
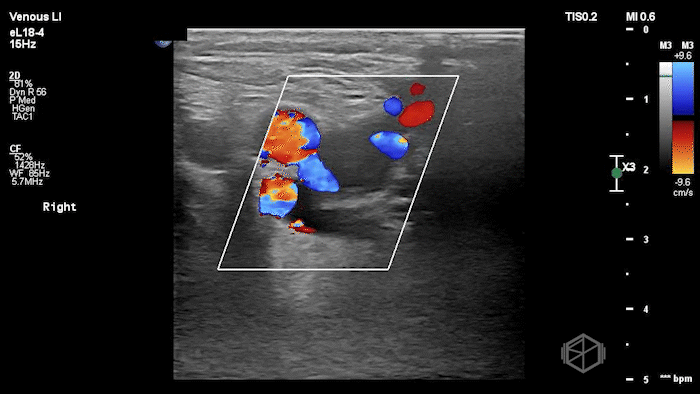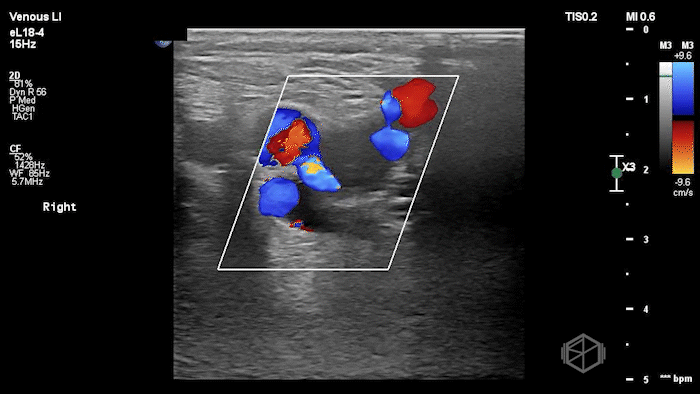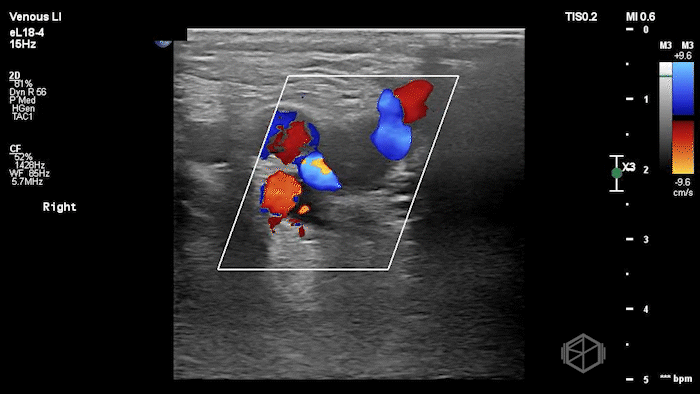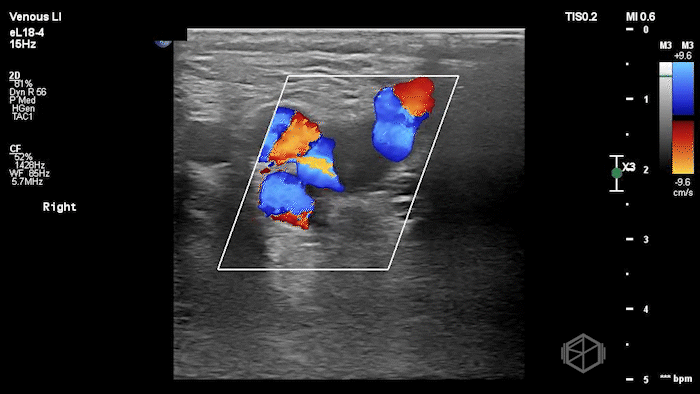
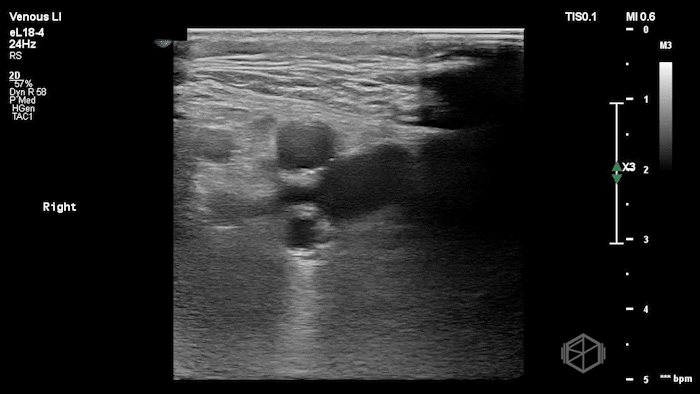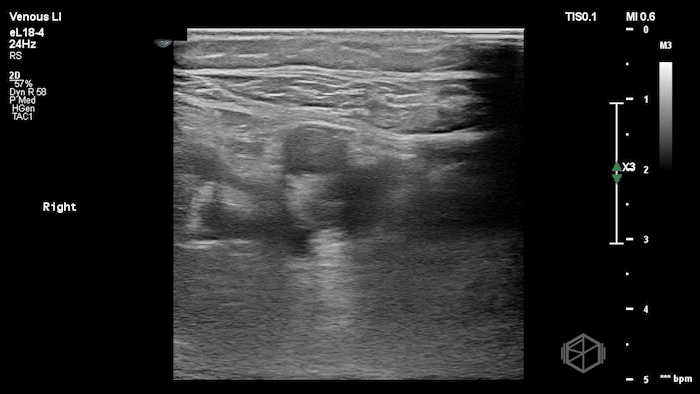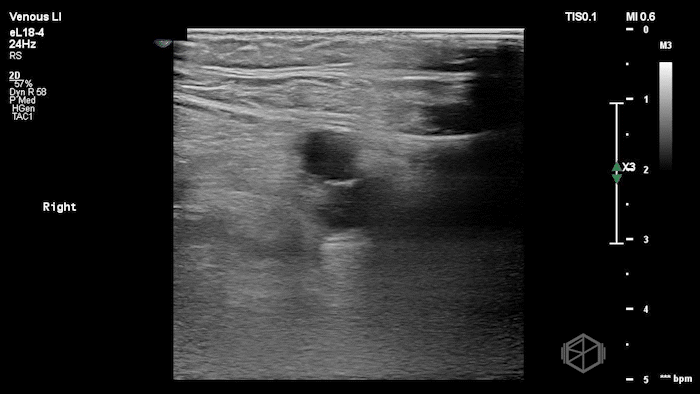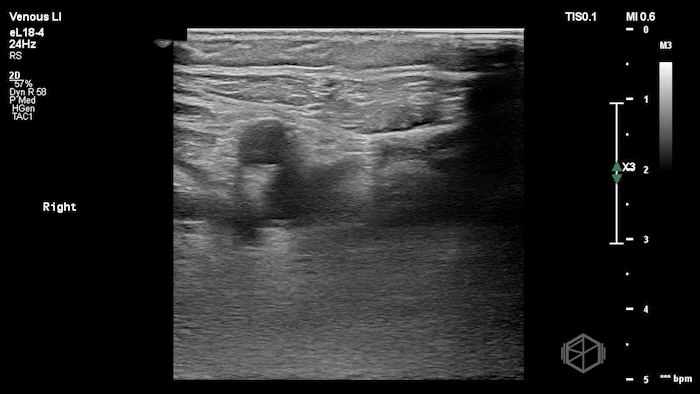
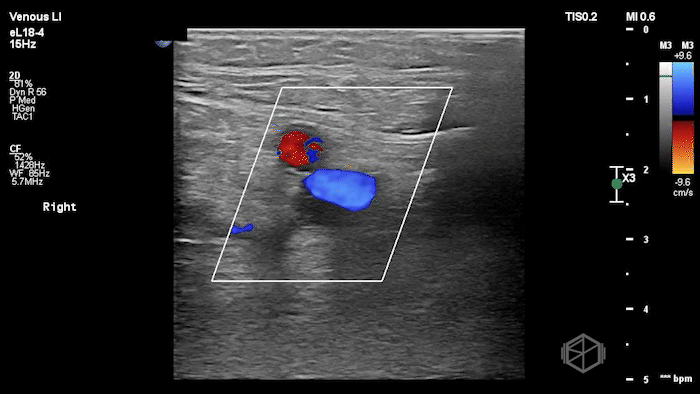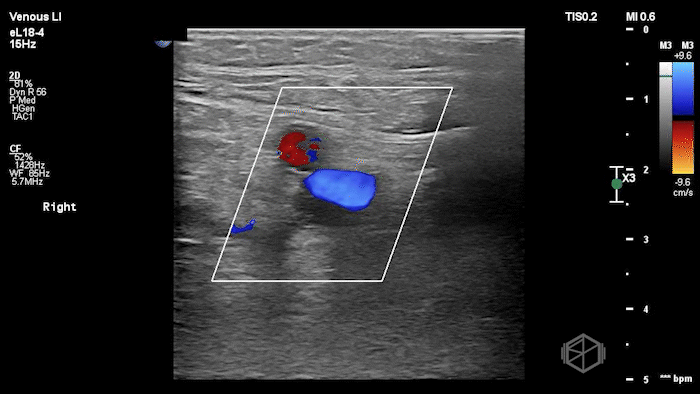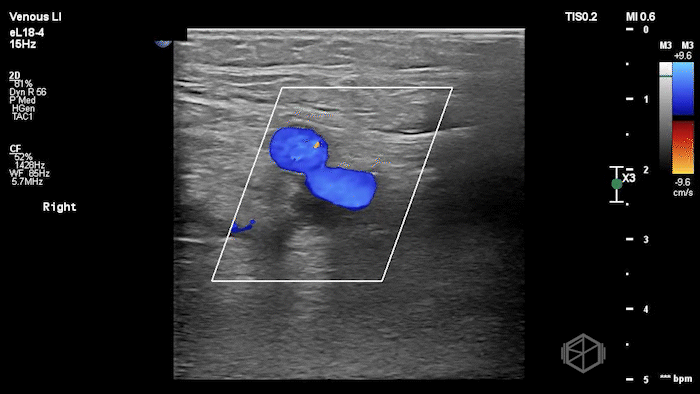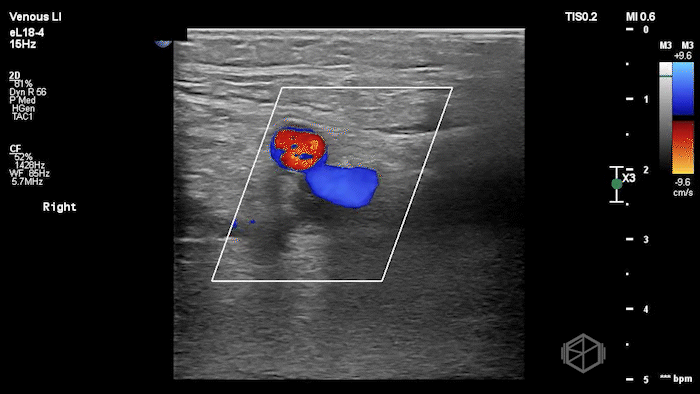
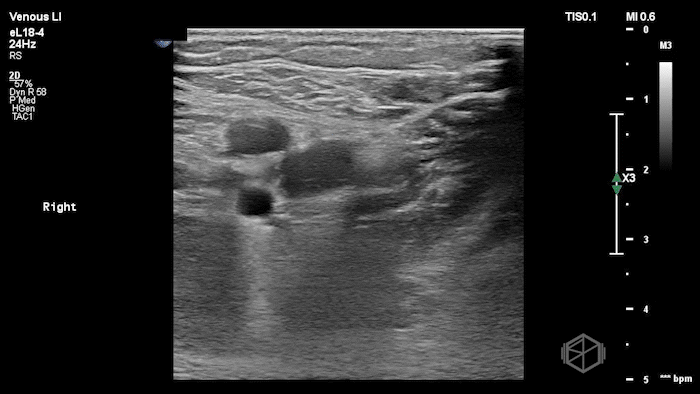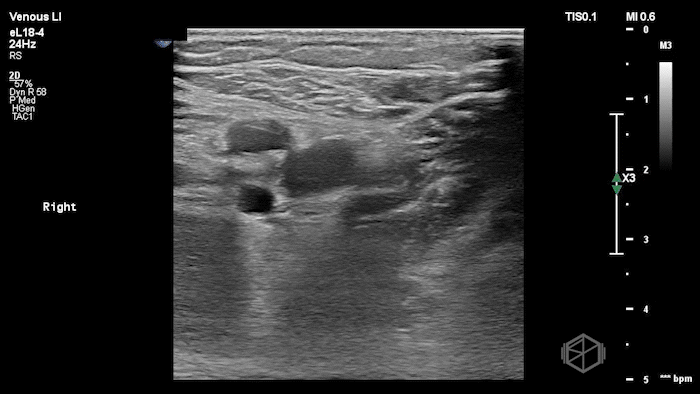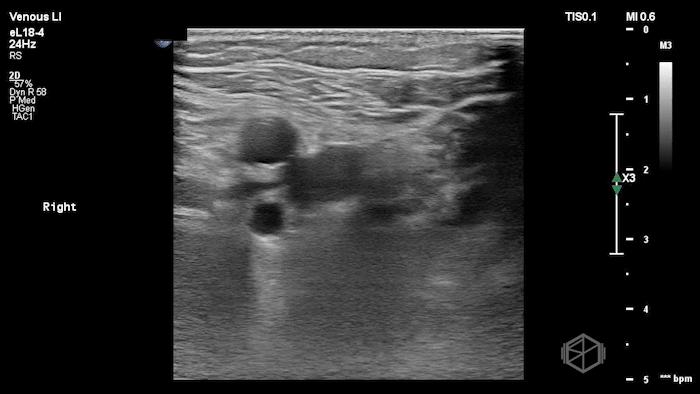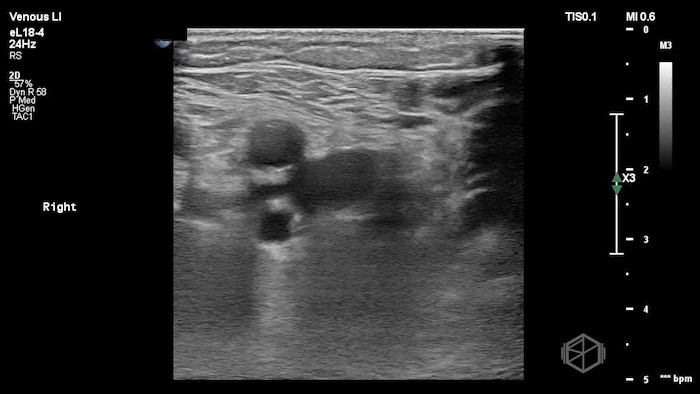
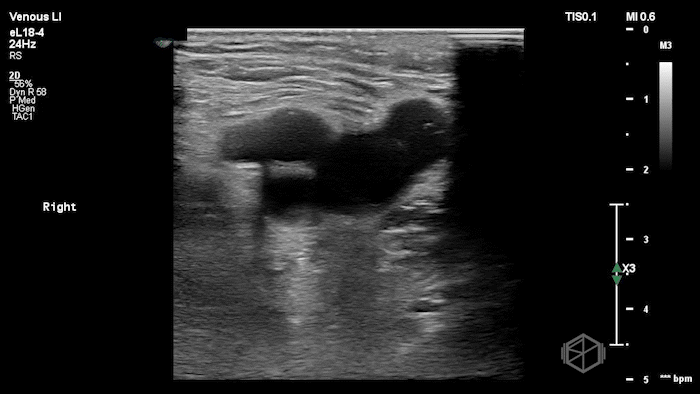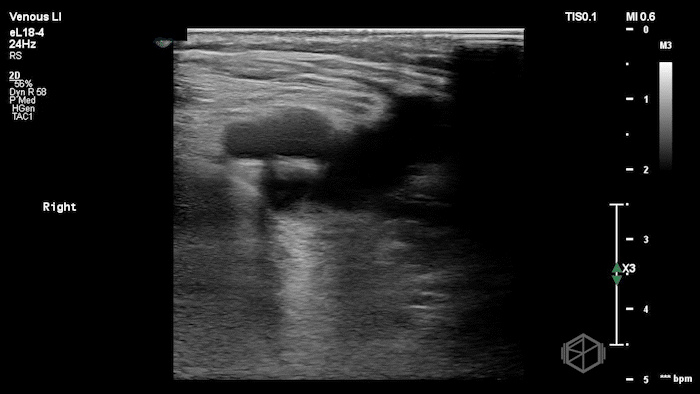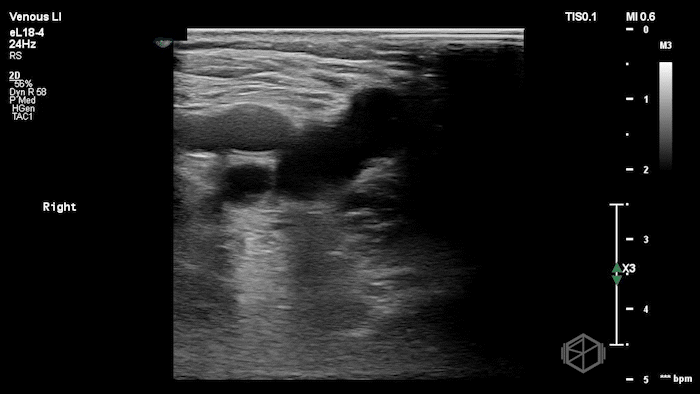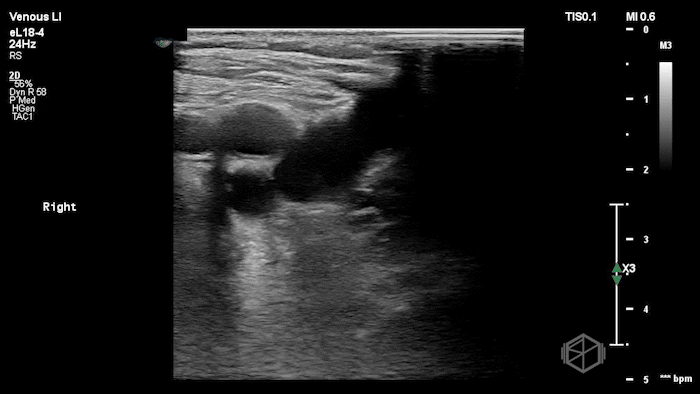
The POCUS shows a right common femoral vein thrombus. Family members reported that the patient had previously been diagnosed with a DVT very recently and was on apixaban.
The thrombus appeared predominantly hypoechoic to nearly anechoic, making it difficult to appreciate on B-mode imaging alone. However, incomplete compressibility of the vein confirmed the presence of thrombus.
Diagnosis: Right common femoral partially occlusive DVT
Learning Points:
Acute DVT may be difficult to visualize on grayscale ultrasound.
Acute thrombus is often hypoechoic or nearly anechoic, which can make it blend with venous blood and difficult to appreciate directly. (📚 PMID: 29261928)
Compression is the key maneuver in DVT ultrasound.
Failure of the vein to fully collapse with probe compression is the most reliable sonographic sign of DVT. (📚 PMID: 11521998)
Acute and chronic thrombi have different ultrasound appearances.
Acute thrombi are typically hypoechoic with venous distension, while chronic thrombi become more echogenic with vein wall thickening and collateral formation. (📚 PMID: 29261928)
POCUS compression ultrasound is highly accurate for proximal DVT.
Compression ultrasound demonstrates ~94–97% sensitivity and ~98% specificity for proximal DVT. (📚 PMID: 16202135)
Multiple POCUS compression ultrasound protocols exist for DVT evaluation.
The two-point exam evaluates the common femoral and popliteal veins, while three-point exams add compression of the femoral vein between the common femoral and popliteal veins.
Extended compression ultrasound (ECUS) evaluates the entire femoral vein from the femoral/deep femoral bifurcation to the adductor canal, helping detect isolated femoral vein thrombi that may be missed by limited protocols. (📚 PMID: 32045437, 31534593, 29610129)
Check out our other SonoProps post for more discussion on lower extremity DVT!
