May SonoProps
Welcome to May!
This month’s first SonoProp goes to Dr. Yianni Flouskakos!
Dr. Flouskakos was caring for a 60-year-old male with a history of multiple medical problems and a known right inguinal hernia who presented to the Emergency Department with right-sided groin pain.
The patient reported a long history of a right inguinal hernia. The day prior to arrival, while driving, he noticed increased swelling and pain in the right groin. He endorsed nausea without vomiting, difficulty voiding his bladder, and pain radiating to his back. His last bowel movement was the day before presentation. He denied fever, chills, chest pain, shortness of breath, abdominal pain, syncope, blood in stool, or diarrhea.
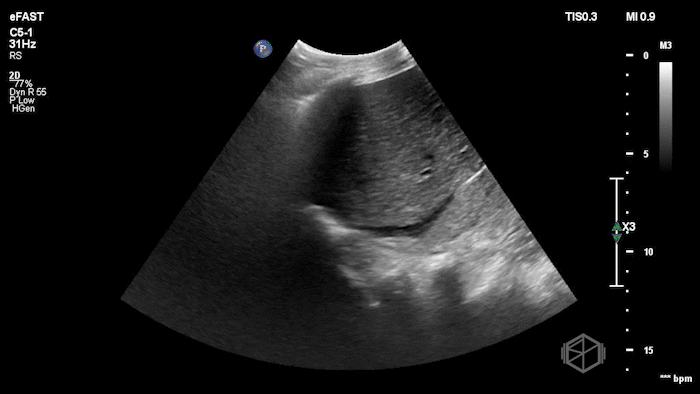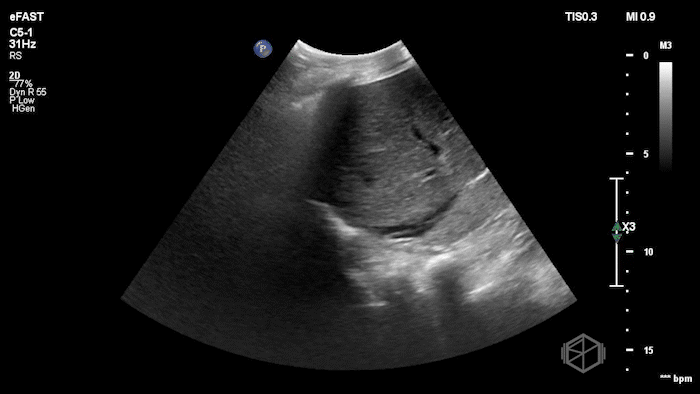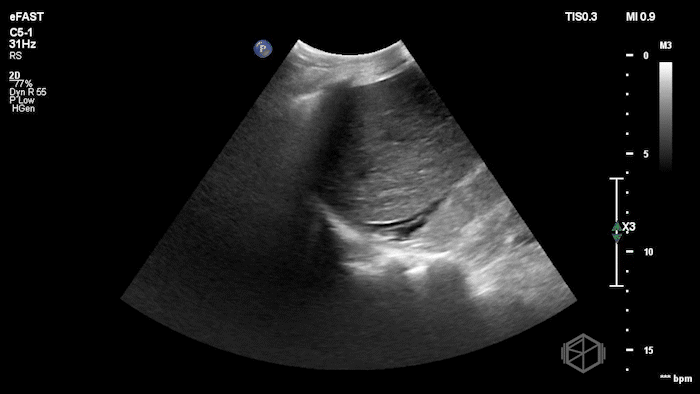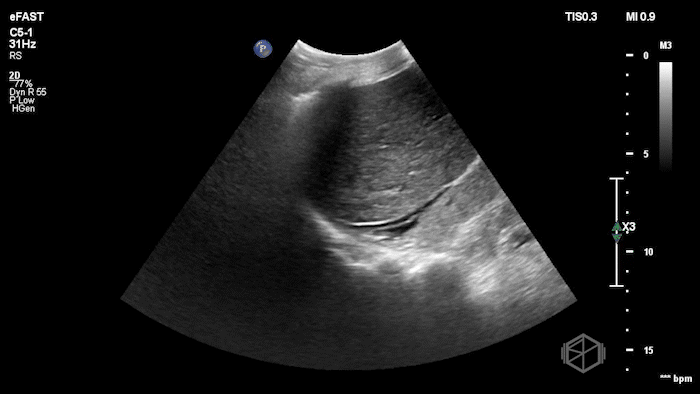
Given the patient’s known hernia with acute worsening pain and swelling, Dr. Flouskakos performed a POCUS of the right inguinal hernia within minutes of the patient’s evaluation.
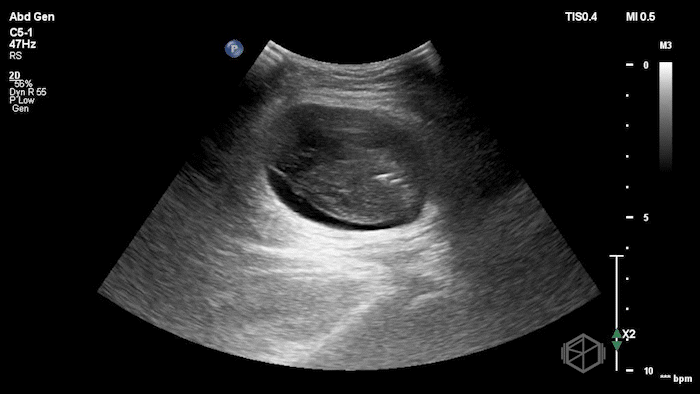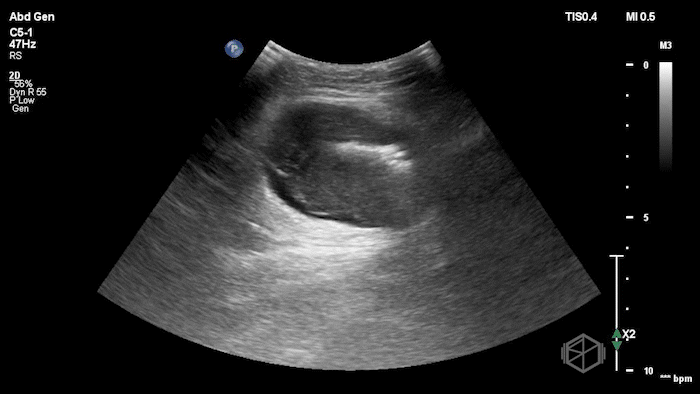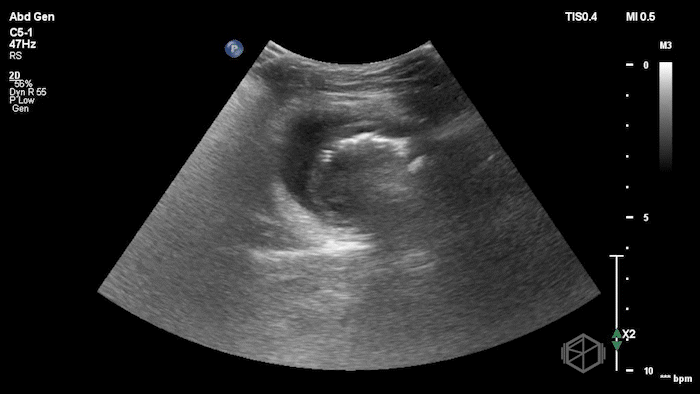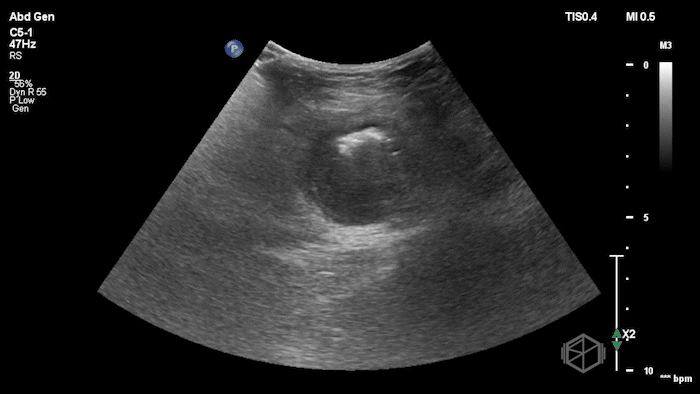
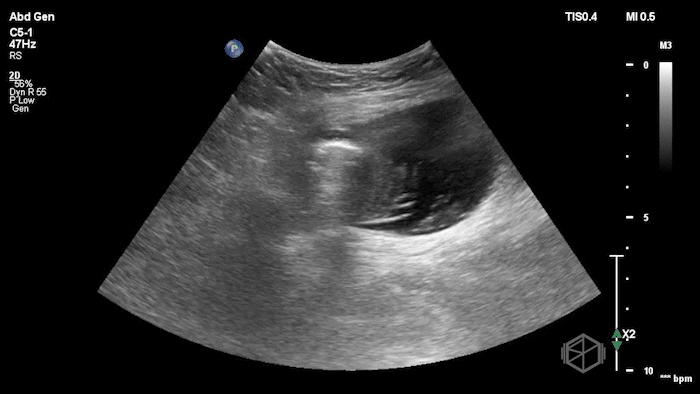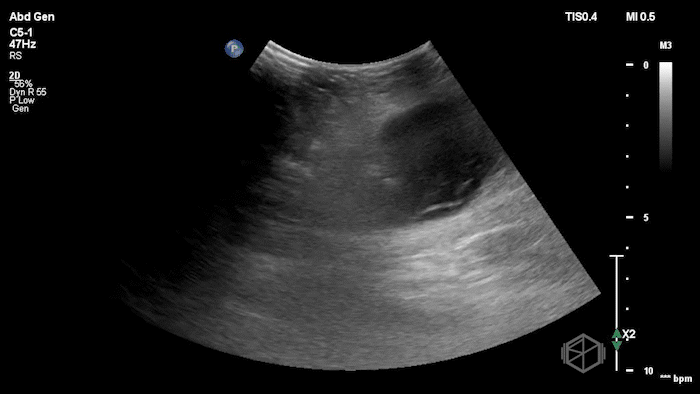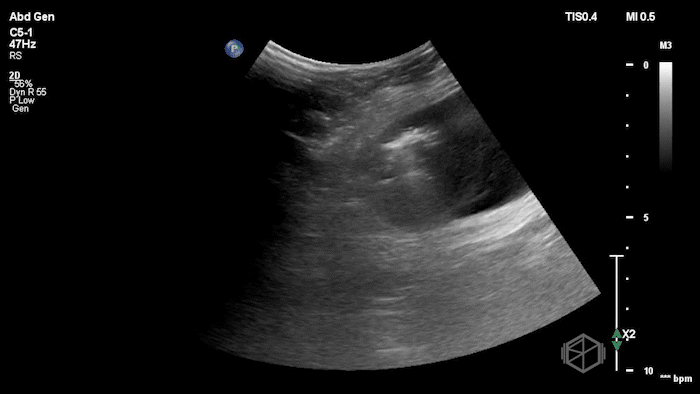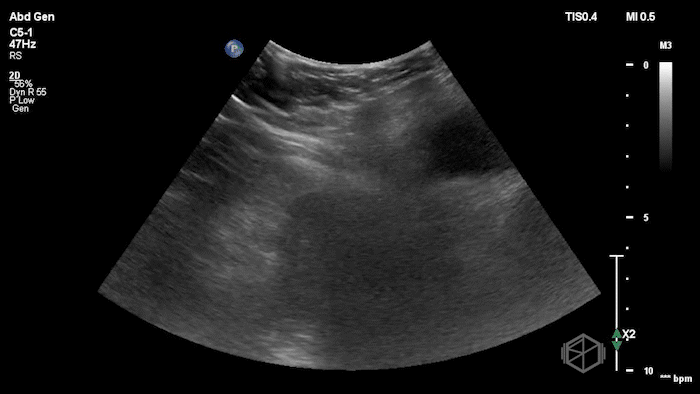
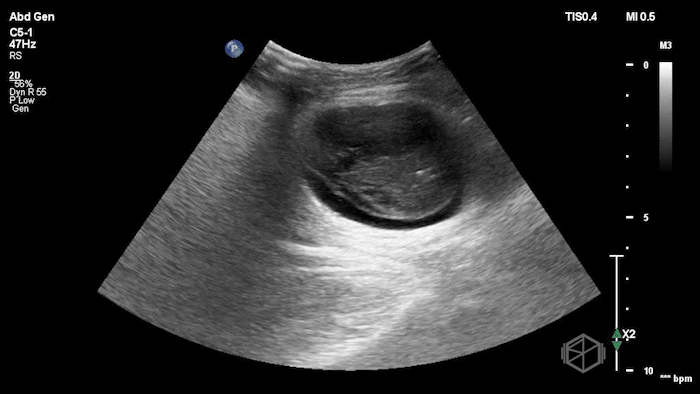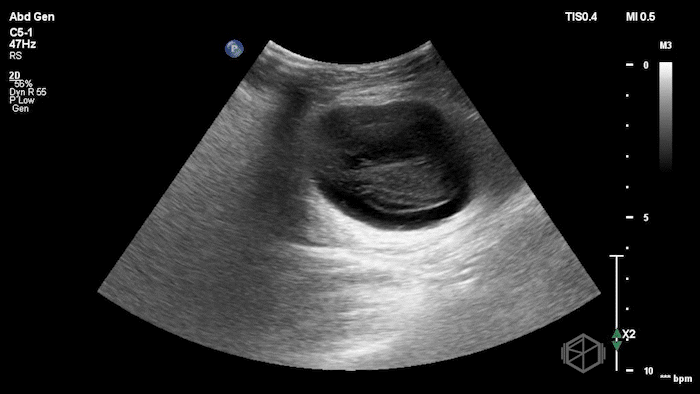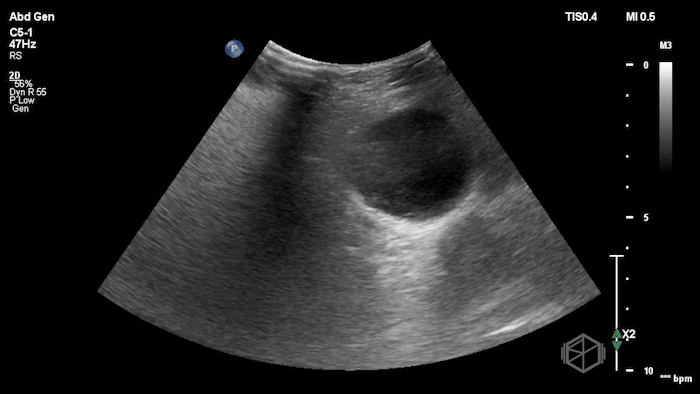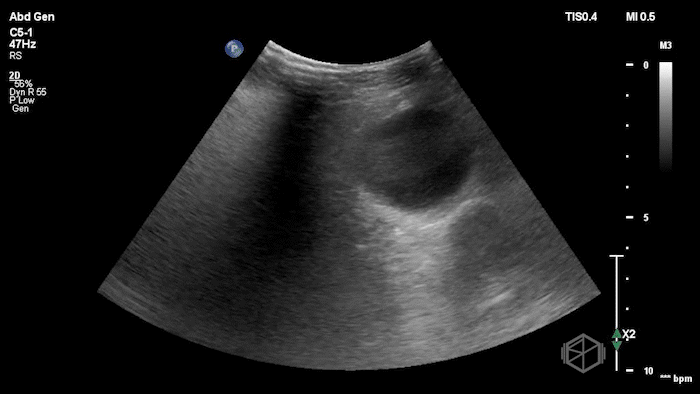
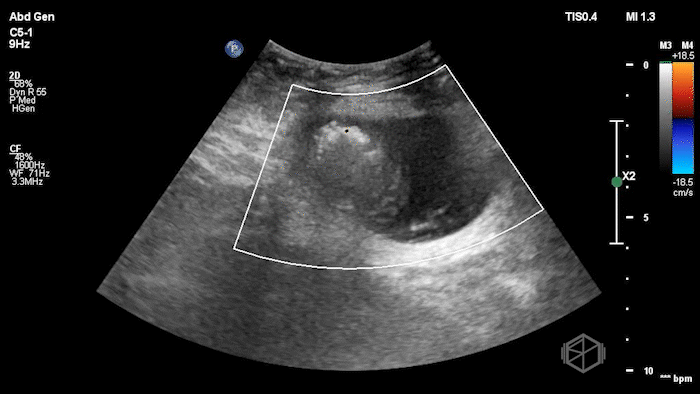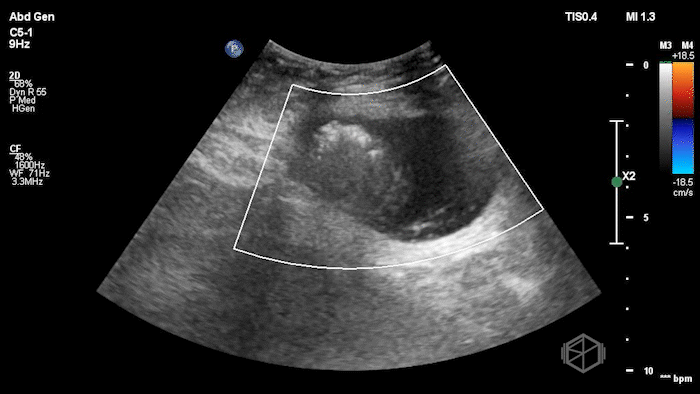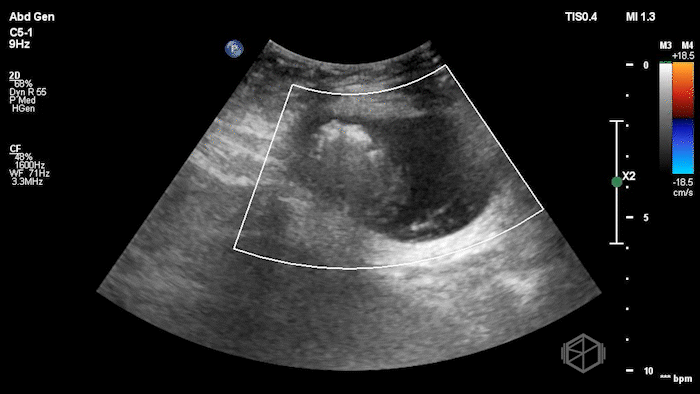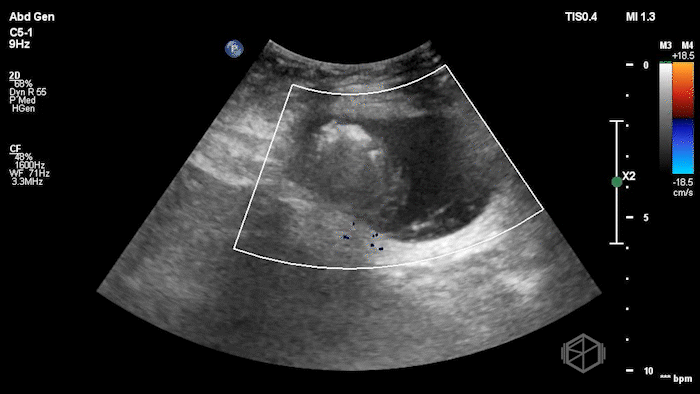
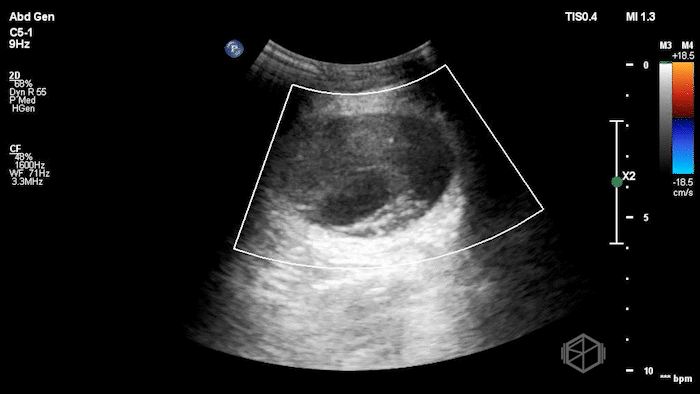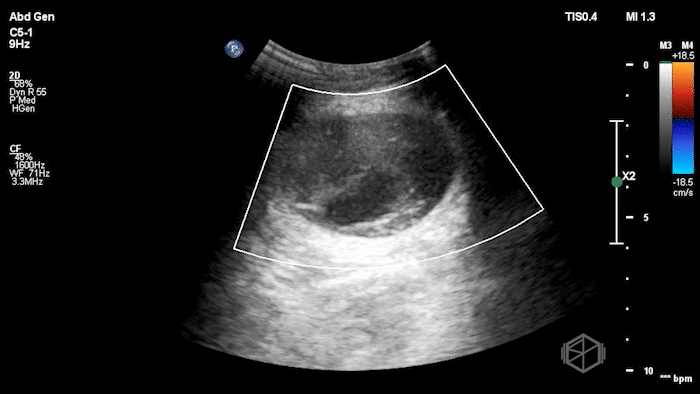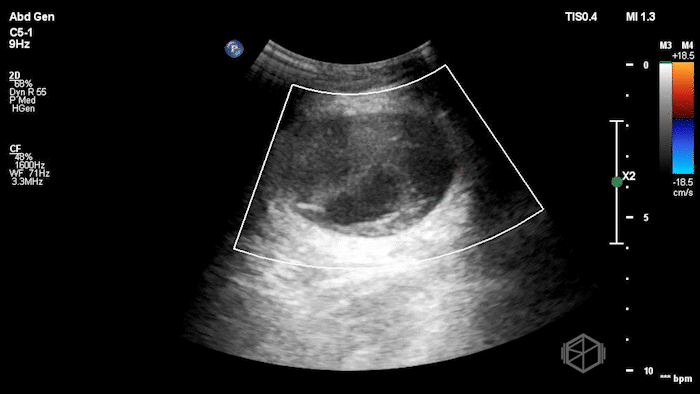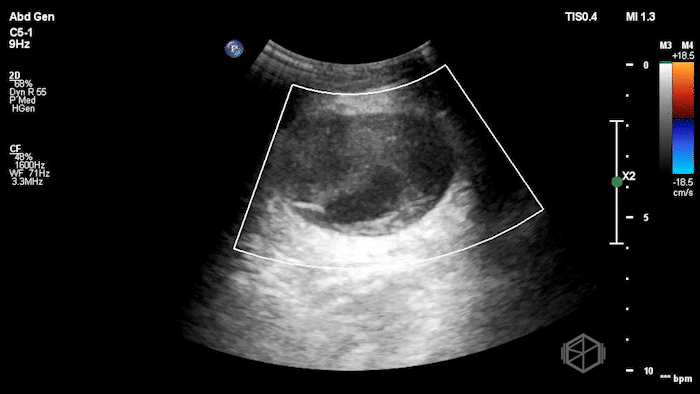
The POCUS demonstrated a right inguinal hernia sac containing bowel. There were tiny reverberation artifacts within the bowel wall, concerning for possible pneumatosis. There was no obvious Doppler blood flow identified within the herniated bowel, raising concern for strangulation. Surgery was consulted shortly after the POCUS exam.
CT abdomen/pelvis later demonstrated a small bowel obstruction with a transition point at the right inguinal hernia, which contained an obstructed loop of jejunum and a portion of the right anterolateral bladder wall. The findings were concerning for strangulation. The patient was taken to the operating room where ischemic bowel was found within the hernia sac. The ischemic segment was resected, a stapled side-to-side anastomosis was performed, and the right inguinal hernia was primarily repaired.
Diagnosis: Right inguinal hernia containing strangulated bowel
Learning points:
POCUS can be a useful bedside tool in the evaluation of suspected incarcerated or strangulated hernias. Findings of a complicated hernia may include bowel or fat within the hernia sac, non-reducible contents, dilated bowel loops, free fluid in the hernia sac, bowel wall edema or thickening, decreased peristalsis, and decreased or absent Doppler flow. In one published case of incarcerated inguinal hernia, POCUS demonstrated a non-reducible inguinal hernia with significant bowel dilation, helping expedite surgical consultation. (📚 PMID: 34377614)
When scanning a painful groin mass, choose the probe that best visualizes the area of concern. A high-frequency linear probe is often useful for superficial groin structures, but a curvilinear probe may provide better depth and field of view depending on body habitus, hernia size, and depth of the sac. Evaluate the hernia sac in two planes, identify the hernia contents, assess for peristalsis, look for free fluid in the hernia sac, and use color Doppler to evaluate bowel wall perfusion. (📚 PMID: 16794175, 17449782, 20823750)
POCUS can help differentiate a reducible hernia from an incarcerated or strangulated hernia. Incarcerated does not always mean strangulated. (📚 PMID: 34377614, 11641170, 35871988)
A reducible hernia may show bowel or fat moving freely through the defect, often with Valsalva or gentle probe pressure.
Incarceration should be suspected when hernia contents are trapped and non-reducible. An incarcerated hernia may still have preserved Doppler flow.
Strangulation should be suspected when there are additional signs concerning for vascular compromise or ischemia, such as absent or markedly decreased Doppler flow, absent peristalsis, bowel wall thickening/edema, or free fluid in the hernia sac. Doppler can be limited by depth, probe pressure, patient motion, and machine settings, so no single POCUS finding should be used in isolation to rule out strangulation. However, absent or markedly decreased Doppler flow in the right clinical context should significantly increase concern for strangulation/ischemia. (📚 PMID: 25987928)
Tiny reverberation artifacts within the bowel wall may represent intramural gas/pneumatosis. In a painful, non-reducible bowel-containing hernia, this should increase concern for ischemic bowel, especially when paired with absent peristalsis or decreased/absent Doppler flow. Pneumatosis is not specific for ischemia, but in the right clinical context it is a high-risk finding. (📚 PMID: 28105581, 10398791, 10874196, 9530294)
POCUS can change the timeline of care. In this case, the patient’s POCUS was performed immediately upon arrival and showed bowel within the hernia sac without obvious Doppler flow. Surgery was consulted right away, before CT resulted about an hour and a half later showing SBO with a transition point at the right inguinal hernia and concern for strangulation. Similar case literature supports POCUS as a tool to rapidly identify complicated hernias at the bedside and expedite operative management. (📚 PMID: 25987928, 35871988)
Our second case also highlights how a quick bedside scan can accelerate care in a hypotensive patient.
The next SonoProps goes to Dr. Rachel Ariz and Dr. Christopher Scavelli.
Dr. Scavelli had a 75-year-old female with a recent admission for renal biopsy complicated by perinephric hemorrhage and anemia requiring blood transfusion, which was later complicated by transfusion-associated circulatory overload. She presented to the Emergency Department with abdominal pain.
The patient reported that in the afternoon she developed upper abdominal pain without a clear trigger. Symptoms started after eating Chinese food, though she was unsure if this was related. The pain remained constant and radiated somewhat to the right upper quadrant and right flank. She denied fever, chills, chest pain, shortness of breath, cough, nausea, vomiting, diarrhea, numbness, tingling, or focal weakness.
On exam, her abdomen was soft with diffuse tenderness to palpation, maximal in the right upper quadrant and right flank. She had no guarding, rebound, or rigidity.
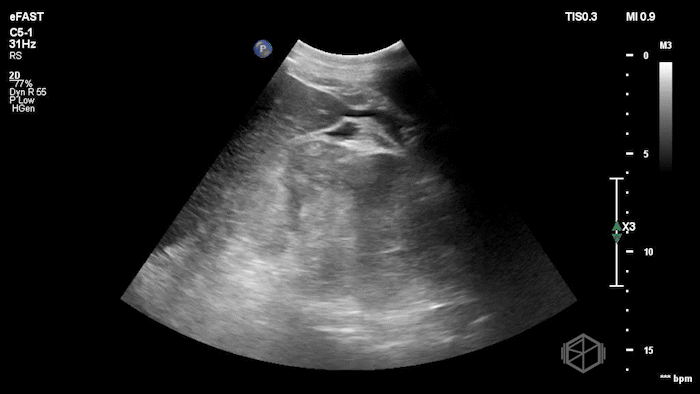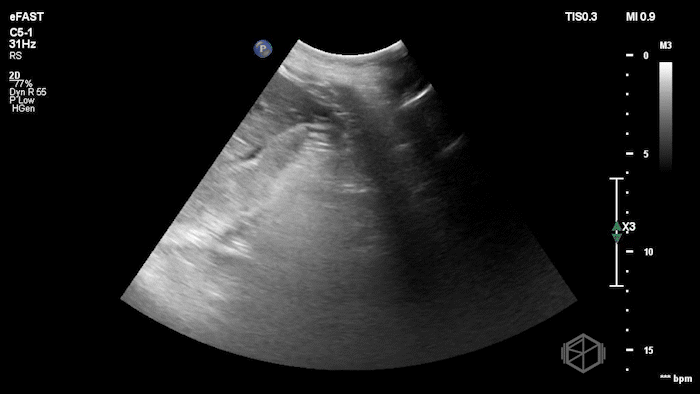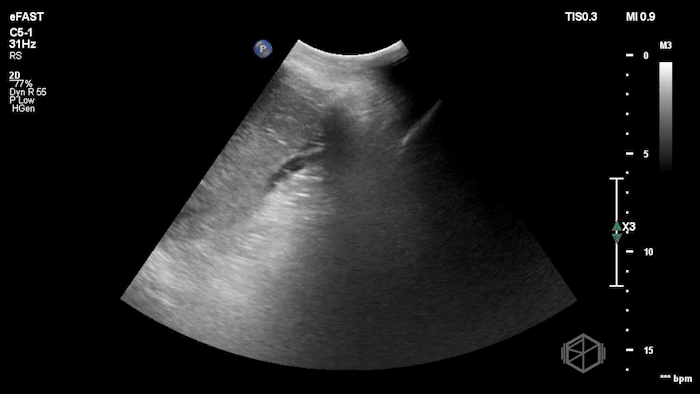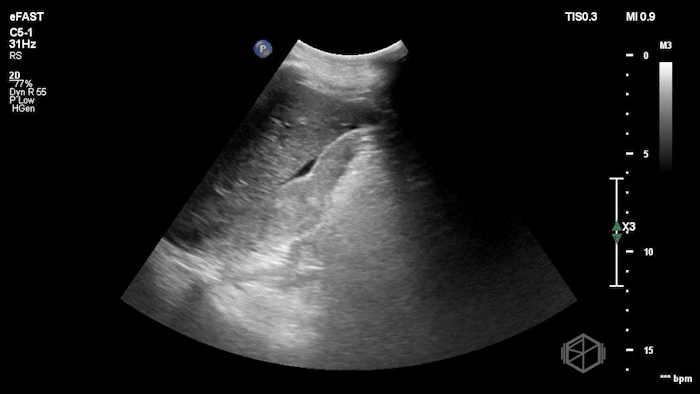
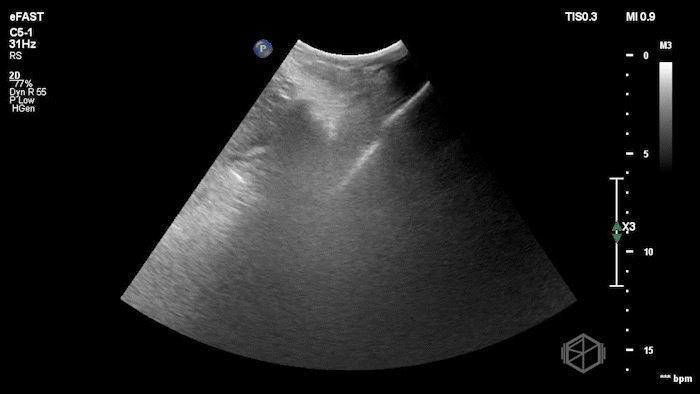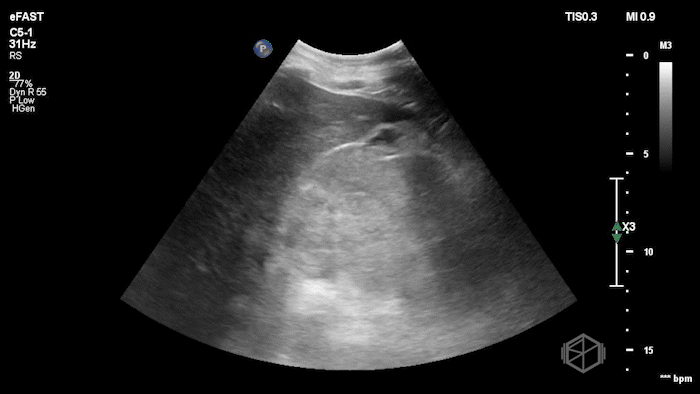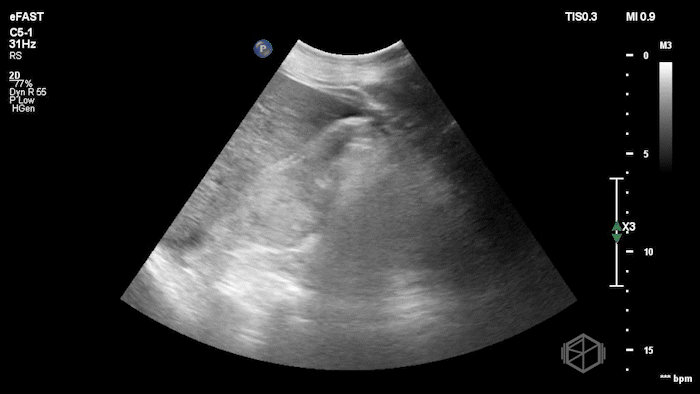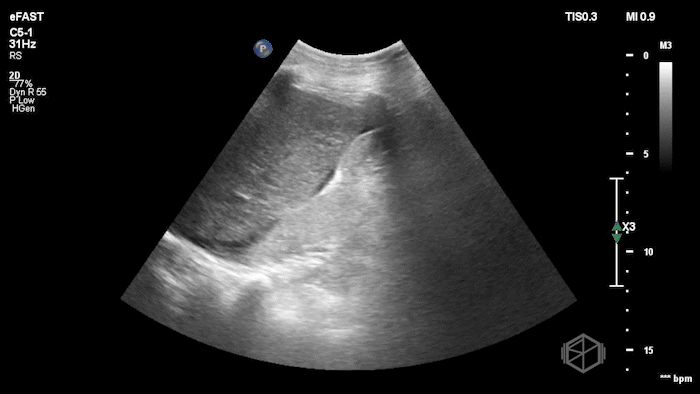
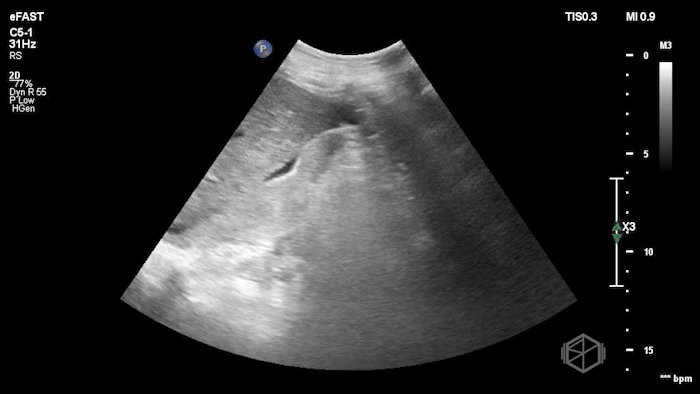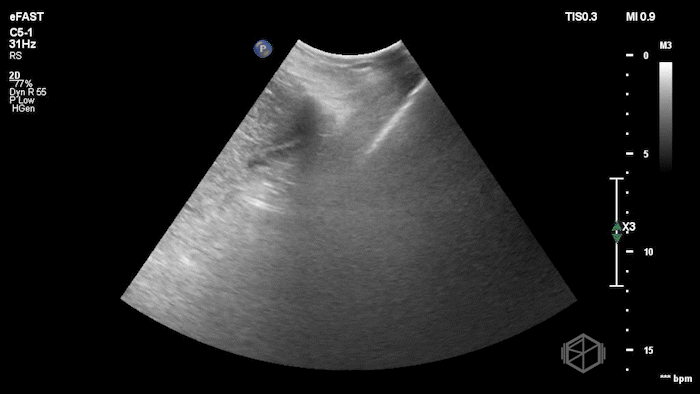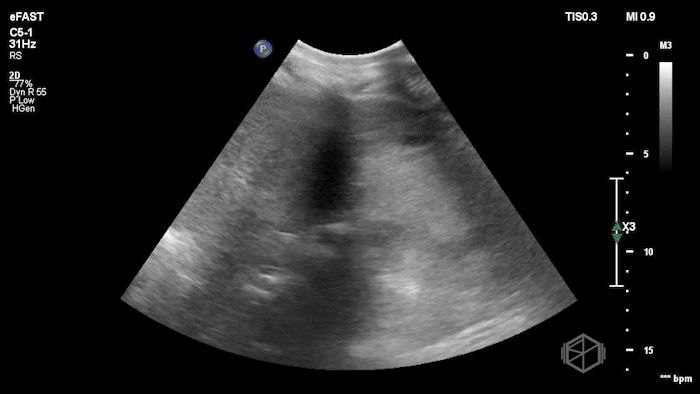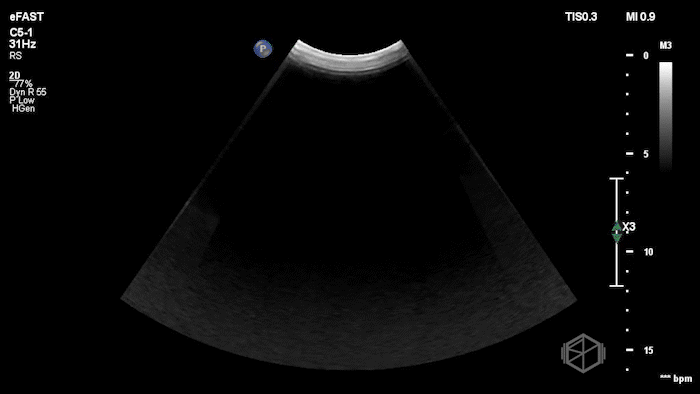
While in the ED, the patient had an episode of hypotension. A FAFF exam was performed by Dr. Ariz and she obtained the following images:
The POCUS demonstrates free fluid near the liver as well as an abnormal-appearing right kidney. Given the patient’s recent renal biopsy, abdominal/flank pain, and hypotension with abnormal POCUS findings, a stat CTA was obtained. CTA showed a large right perirenal hematoma with active hemorrhage and possible small pseudoaneurysm within the lower pole of the right kidney.
The patient was taken emergently to Interventional Radiology. Angiography demonstrated several bleeding foci arising from one of the right renal arteries, including a dominant lower pole pseudoaneurysm. The involved vascular territory was embolized with dilute glue.
Diagnosis: Active hemorrhage from right renal artery pseudoaneurysm after renal biopsy, prompted by abnormal FAFF/renal POCUS
Learning points:
POCUS can be a useful bedside tool in undifferentiated hypotension, especially when the history points toward hemorrhage. In this case, recent renal biopsy, abdominal/flank pain, and intermittent hypotension made recurrent perinephric or retroperitoneal bleeding a key concern. POCUS identified the abnormal RUQ free fluid and an abnormal-appearing kidney, prompting stat CTA and IR involvement.
Bleeding is the most common complication of percutaneous renal biopsy. Post-biopsy bleeding may present as perinephric hematoma, retroperitoneal hemorrhage, hematuria, anemia, flank/abdominal pain, hemodynamic instability, or need for transfusion or intervention. Renal artery pseudoaneurysm is an uncommon but important vascular complication that may present with delayed or recurrent bleeding after biopsy. (📚 PMID: 31123379, 33708800, 19814646)
When scanning the kidney after recent biopsy, look for perinephric fluid or hematoma, distortion of the renal contour, echogenic clot, mass effect on the kidney, and interval change compared with prior imaging when available. Color Doppler may help identify vascular complications such as pseudoaneurysm or arteriovenous fistula, but lack of an obvious Doppler abnormality should not exclude active bleeding when the clinical picture is concerning. (📚 PMID: 36896114, 19246472)
FAST/FAFF can detect intraperitoneal free fluid, but it is limited for retroperitoneal hemorrhage. A negative FAST should not reassure the clinician when retroperitoneal bleeding remains high on the differential. In the right clinical context, a positive RUQ view should accelerate definitive imaging, with CTA used to characterize the hematoma, localize active bleeding, and guide IR management. (📚 PMID: 30853094, 21641153)
POCUS can change the timeline of care. In this case, hypotension prompted a bedside FAFF exam showing free fluid near the liver and an abnormal right kidney. CTA then demonstrated a large right perirenal hematoma with active hemorrhage and possible pseudoaneurysm, and the patient underwent emergent renal artery embolization. Significant post-biopsy bleeding complications can often be treated with angiography and selective or superselective embolization. (📚 PMID: 24004870, 19814646, 19589577)