February SonoProps
February brings Valentine’s day as well as another edition of SonoProps! This month was extremely tough as we had some amazing scans and made it very hard to choose. But in the interest of keeping things varied we must pick only two winners with topics not covered previously.
The first of our SonoProps goes to Dr. Marina Frayberg our resident rotator for the block.
She was scanning a 75-year-old male with a history hyperlipidemia, hypertension, Barrett's esophagus, chronic smoking who presented to the ED with shortness of breath. He had not seen a doctor in a long time and was noted to have bilateral lower extremity swelling.
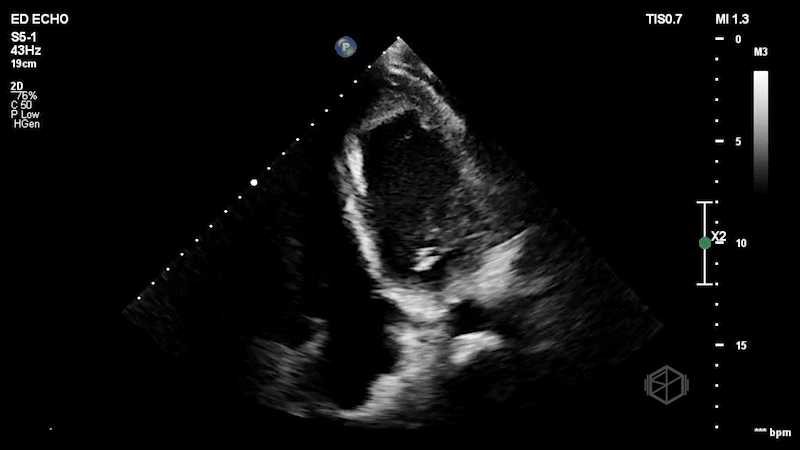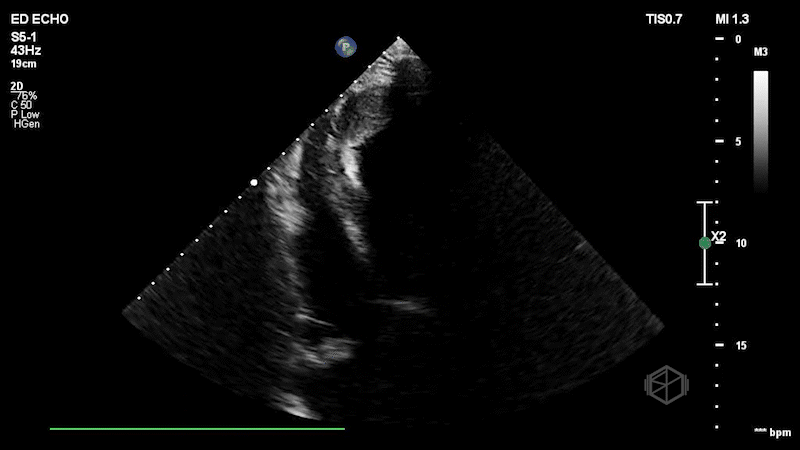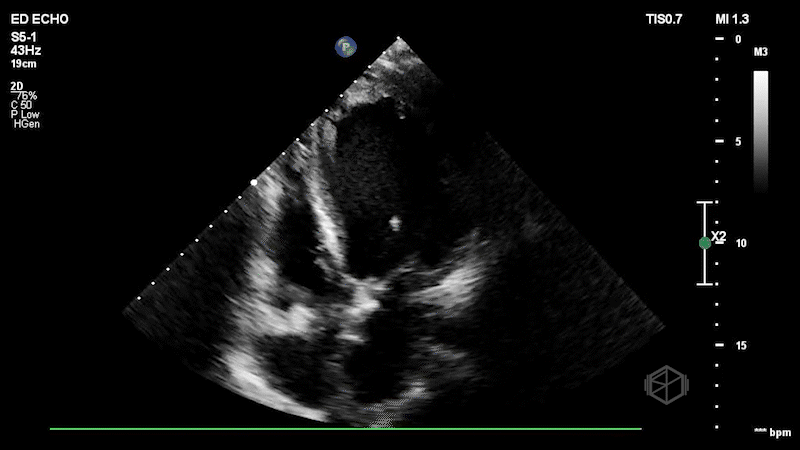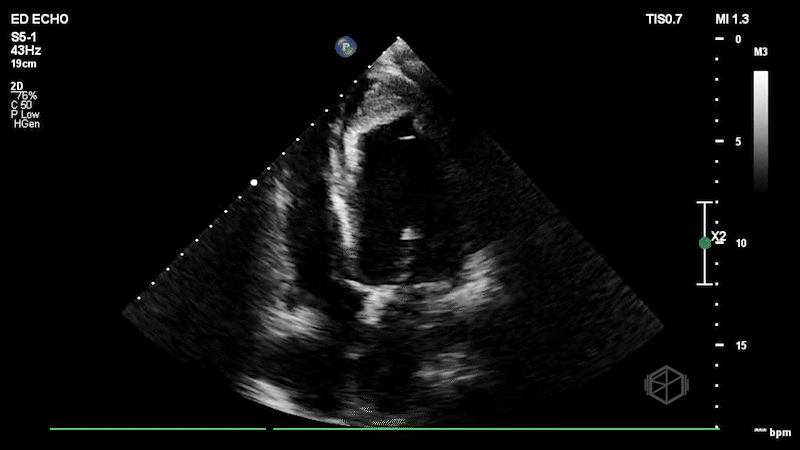
Dr. Frayberg saw this on her echo:
This patient has a significantly reduced ejection fraction, around 15%, with a heterogenous appearing mass at the apex of the left ventricle consistent with an apical thrombus. Normally contrast is used to see apical thrombi but since this was so large it was fairly obvious the patient had an LV thrombus.
Diagnosis: Heart failure with reduced ejection fracture, large apical thrombus
Learning points:
Shortness of breath with lower extremity swelling should prompt a POCUS for evaluation for the underlying etiology such as heart failure. This patient had no known diagnosis of LVEF and because a POCUS was performed, his diagnosis was significantly expedited. Cardiology was brought on board early, and the patient was admitted to CCU.
Thrombus may develop in any cardiac chamber, especially those with low pressure and low flow (31074225). The pathophysiology can be attributed to 3 potential factors (1) stasis attributable to reduced ventricular function, (2) endocardial injury, and (3) inflammation/hypercoagulability. In this case it was likely due to stasis due to the patient’s globally reduced LV function.
Thrombi can be hyperechoic, isoechoic, or hypoechoic. A thrombus is usually homogenous with irregular borders and fills in the apex of a ventricle or attaches to the chamber wall or valves of atria.
Transthoracic echo is usually enough to detect ventricular thrombus. Echo contrast may be used to delineate ventricular borders and identify a thrombus easier.
Contrast echo showing apical LV thrombus.
The second of this month’s SonoProps goes to Dr. Hardeep Singh and Dr. Randye Bernot.
They were taking a 76-year-old female who presented to the ED with abdominal pain, initially in the right lower quadrant which moved to the right upper quadrant. The patient had gone to an urgent care where she had a chest X-ray that was negative and was sent to a Cardiologist who did some labs and an EKG that were negative so they sent the patient to the ER. The patient had some right upper quadrant tenderness without Murphy’s sign.
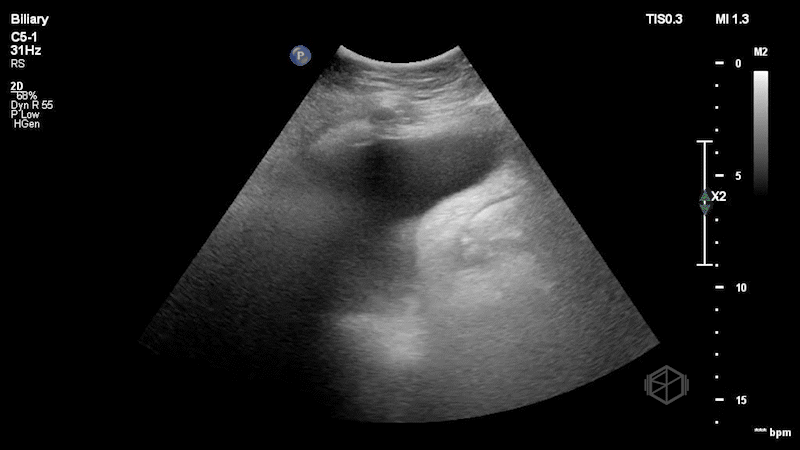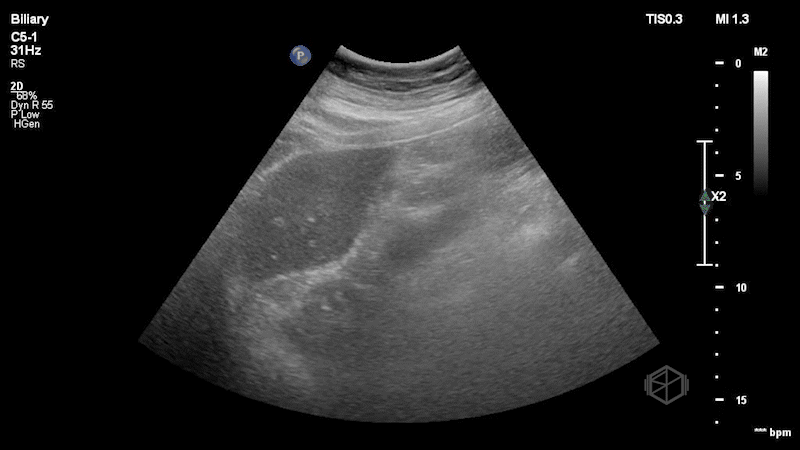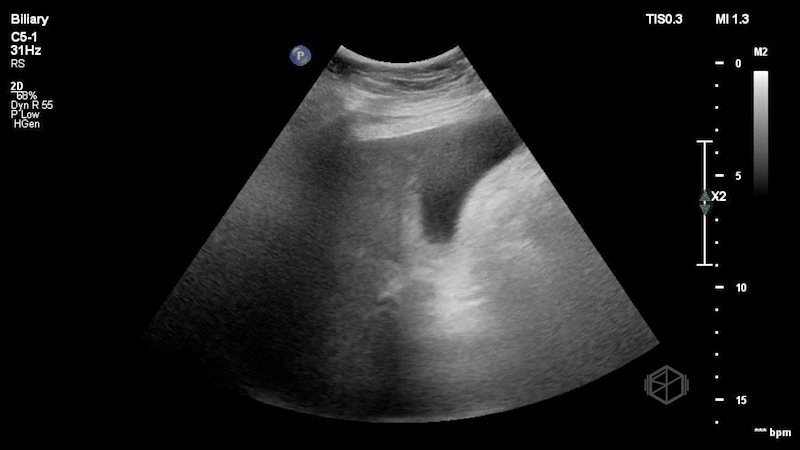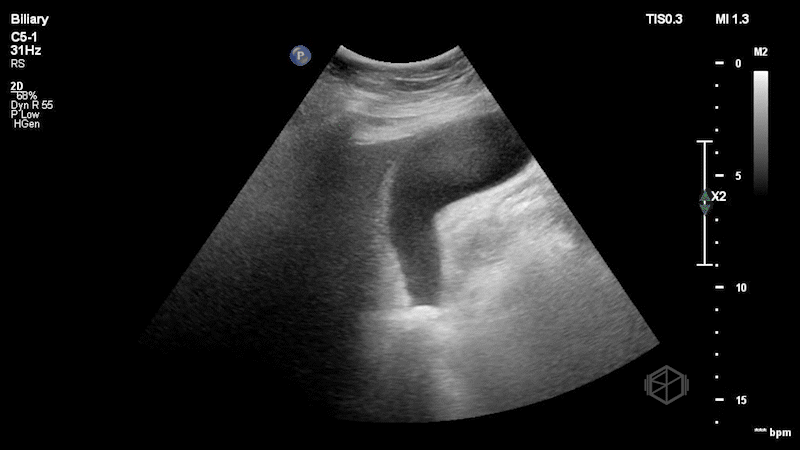
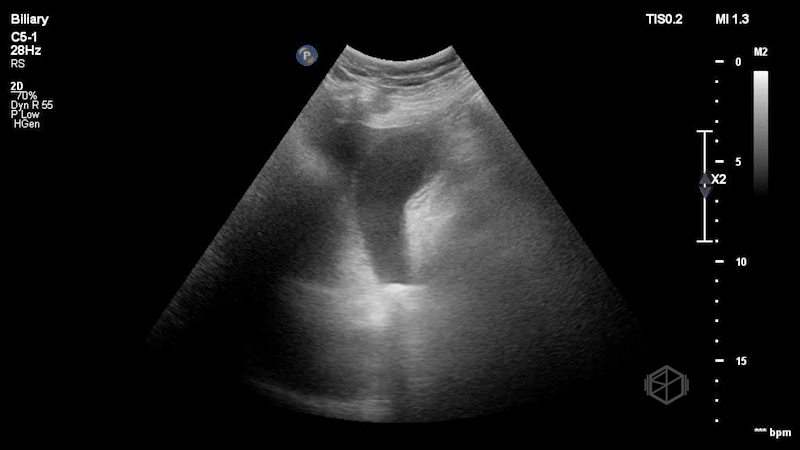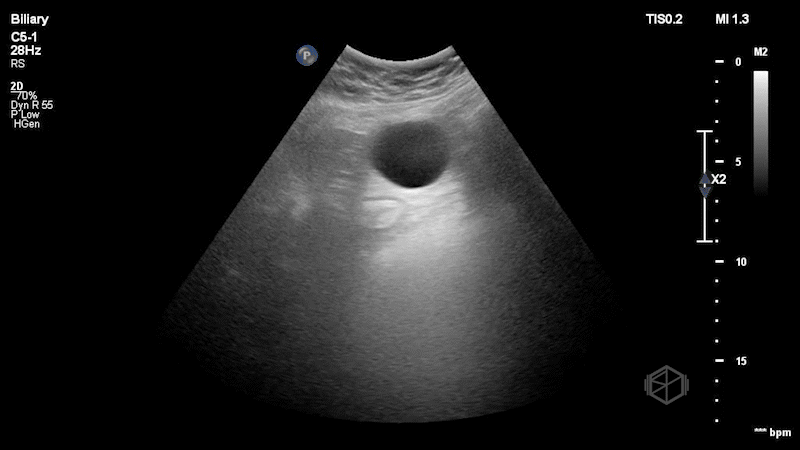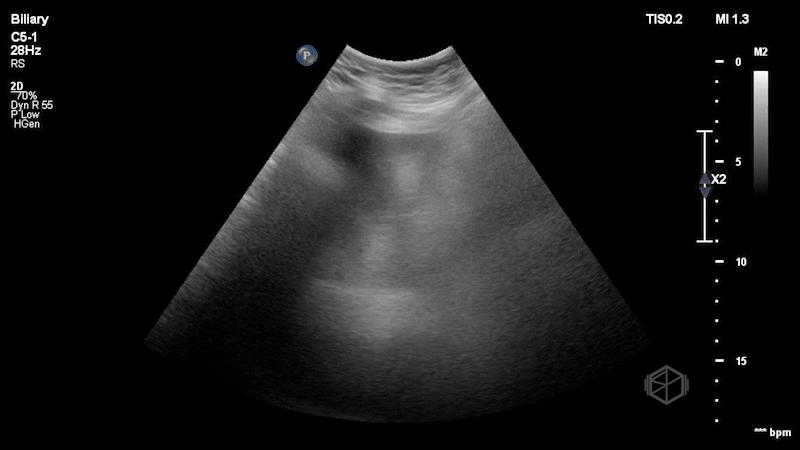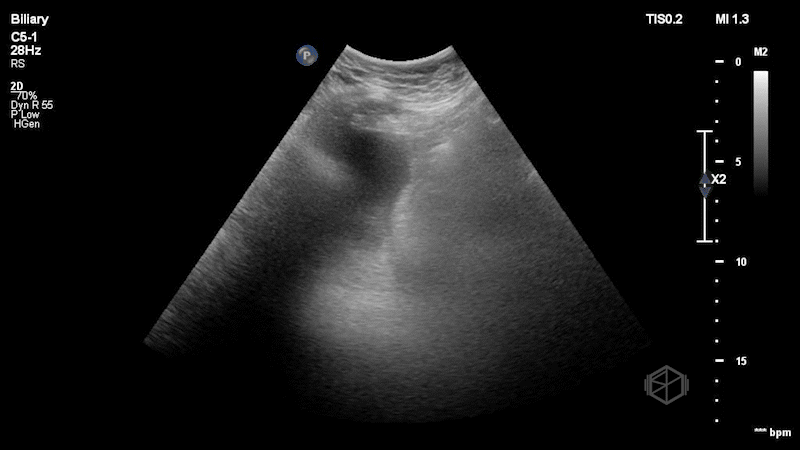
Dr. Singh and Dr. Bernot immediately grabbed the ultrasound and performed the following scan:
This is a great scan that highlights the difficulty of biliary sonography and some provides some key teaching points. This gallbladder is elongated with a very subtle stone--in-neck. The patient had a radiology ultrasound that demonstrated “Distended fluid-filled gallbladder with 1.5 cm echogenic shadowing nonmobile gallstone in the gallbladder neck which does not move on decubitus imaging. No pericholecystic fluid.” There was no sonographic Murphy’s sign. The patient was taken to the OR where the gallbladder was noted to be hydropic and acutely inflamed.
Diagnosis: Stone-in-neck Sign (SIN), acute cholecystitis
Learning points:
It is very important to visualize the neck of the gallbladder. This is a place where many stones are missed.
If you do not see the neck of the gallbladder, the scan is limited and there must be further imaging performed if there is high suspicion for cholelithiasis or cholecystitis.
A stone may be identified based on shadowing. This must also be differentiated from edge artifact, although edge artifact will usually disappear with probe movement while shadowing will persist.
SIN sign is defined as an immobile stone lodged in the neck of the gallbladder. The stone must be lodged in the neck of the gallbladder and should not move when the patient is turned. There should be no anechoic spaces between the stone and the neck of the gallbladder.
SIN has a specificity of 97% and a positive predictive value of 93% in diagnosing cholecystitis. If there is an impacted stone in the neck of the gallbladder, even without other five signs of cholecystitis, a surgical consult should be obtained.