January SonoProps
Happy New Year everyone!
The first of this month’s SonoProp goes to Dr. Marina Frayberg with Dr. Jessica Harmon.
Dr. Harmon had an 87-year-old female with a significant past medical history of heart failure with preserved ejection fraction (HFpEF), mitral regurgitation, coronary artery disease, chronic kidney disease, who presented to the ED with shortness of breath saturating 85% on room air.
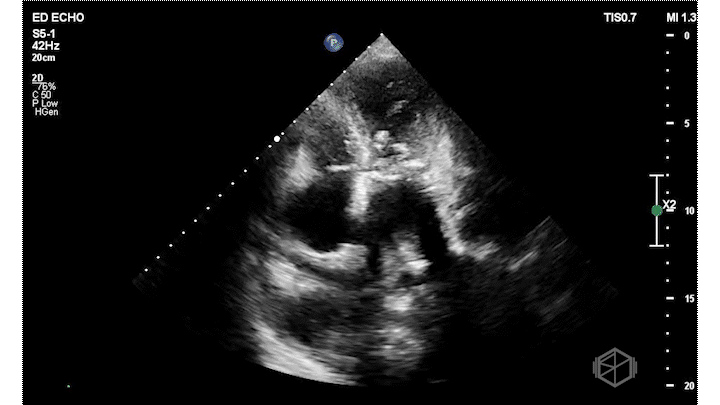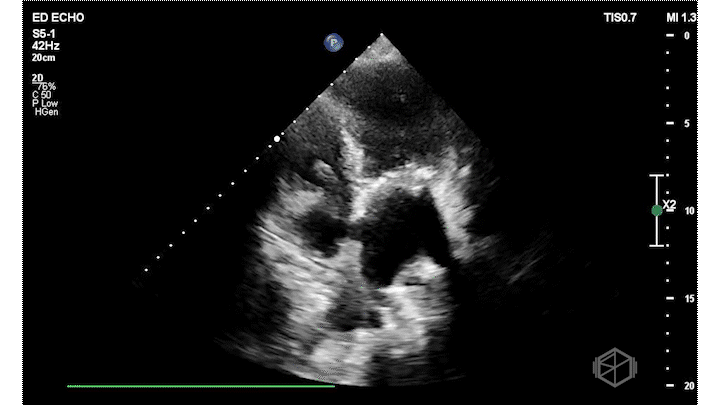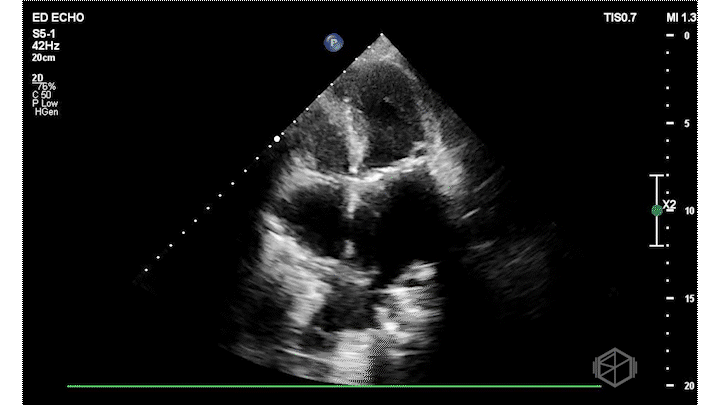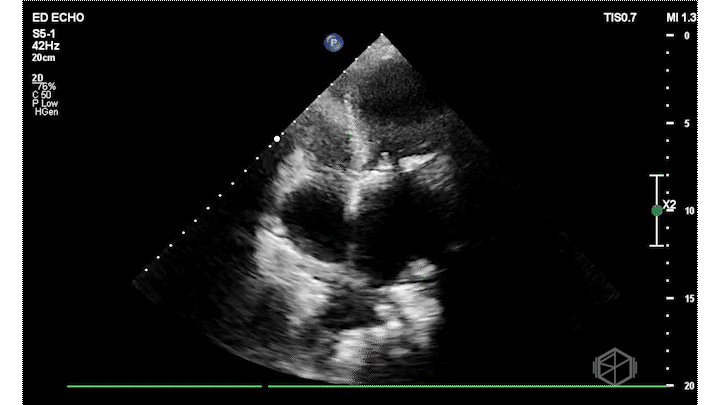
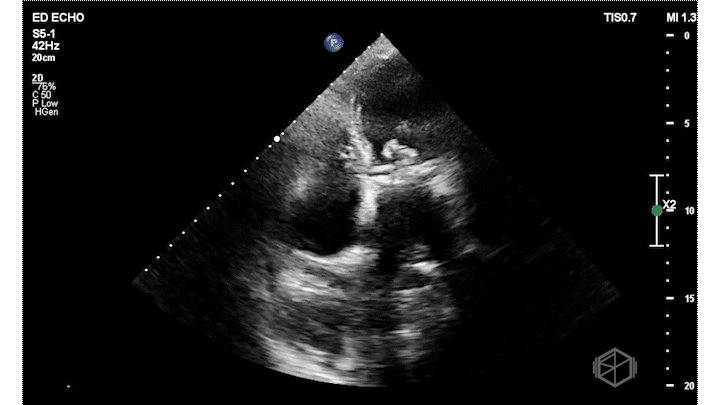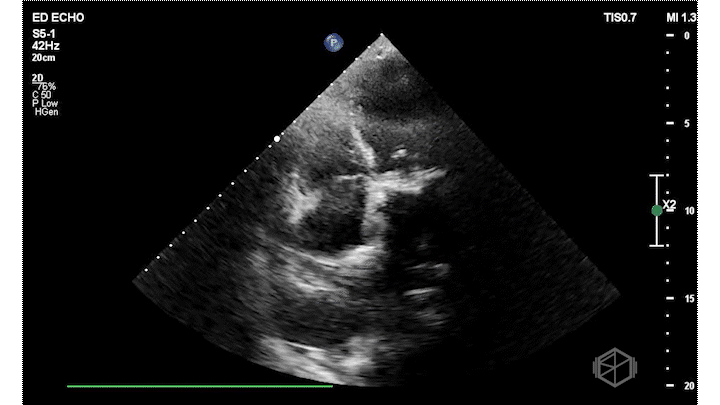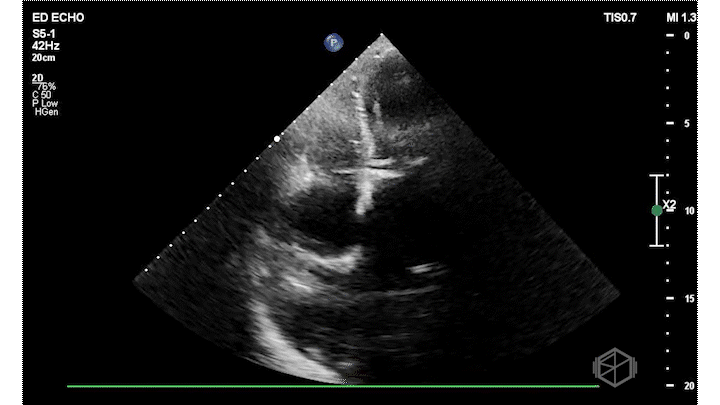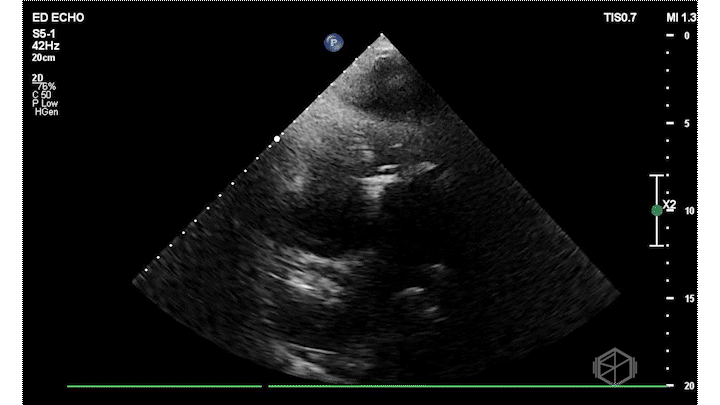
Dr. Frayberg did an echo that showed the following:
The ejection fraction appears grossly normal. There is no pericardial effusion. The right ventricle appears normal size at least in these views. The mitral valve has a very hyperechoic density: severe mitral annular calcification (MAC). There is also a pleural effusion. The patient was admitted for heart failure and acute hypoxic respiratory failure.
Diagnosis: Severe MAC, HFpEF
Learning points:
MAC is found incidentally a majority of the time and requires no specific treatment other than evaluation and modification of cardiac risk factors.
MAC is associated with atherosclerotic disease and negative cardiovascular outcomes. If MAC is present, consider coronary artery disease and address modifiable risk factors (HTN, HLD) (26493666).
Patients with MAC often have HFpEF related to left ventricular diastolic dysfunction and if symptomatic with HF need diuretic therapy (34240401).
MAC can be associated with mitral regurgitation, less commonly mitral stenosis, stroke from increased atrial fibrillation due atrial remodeling, infective endocarditis (S. aureus most commonly attaching to calcific deposits), and increased mortality based on severity (35953138).
It difficult to differentiate between MAC and vegetations. Typically, MAC will cast a shadow and is found at the annulus, making it easier to identify. In contrast, vegetations are usually more mobile and do not cast shadows. If unsure, you can note that there is a hyperechoic density on the mitral valve that likely indicates MAC. (33172308).
The second SonoProps goes to Dr. Ahmer Salman.
Dr. Salman was scanning a 40-year-old pregnant female who had presented to the ED a few days prior for vaginal bleeding in pregnancy and had an ultrasound that at that time showed a single intrauterine pregnancy with crown-rump length of 0.6 cm projecting to 6 weeks 3 days. No fetal cardiac activity was detected. Findings are suspicious but not definitive for pregnancy failure.
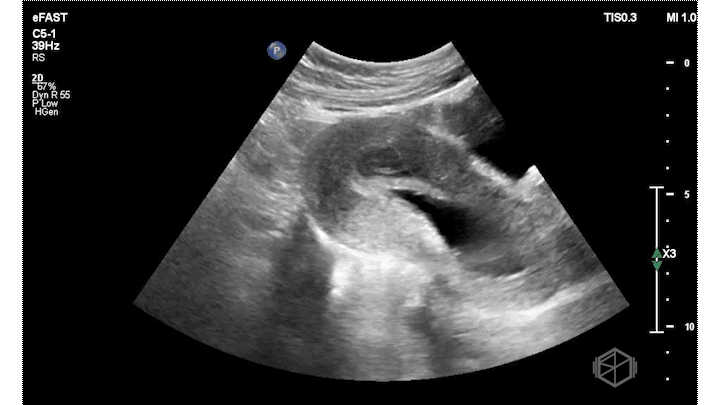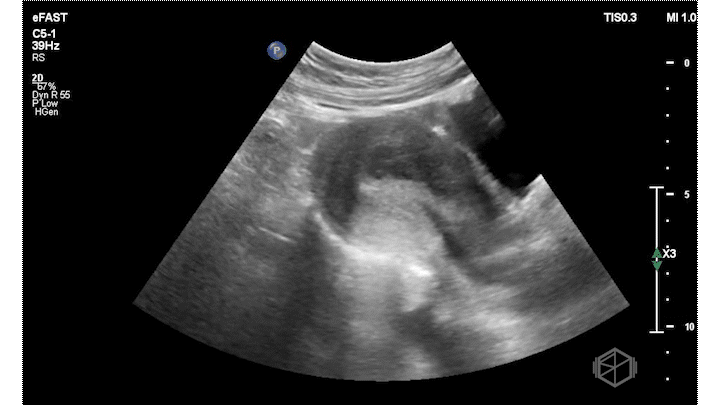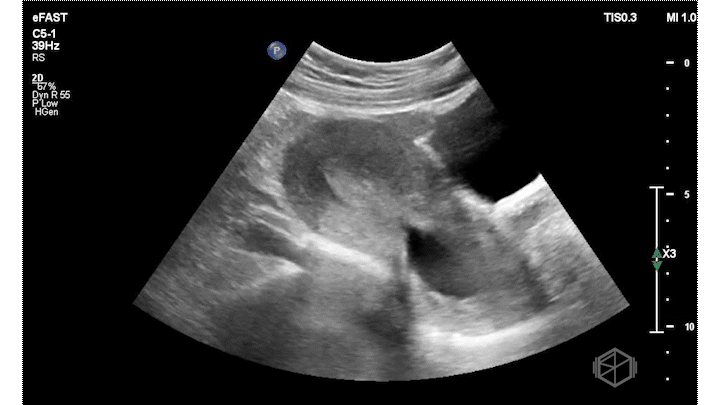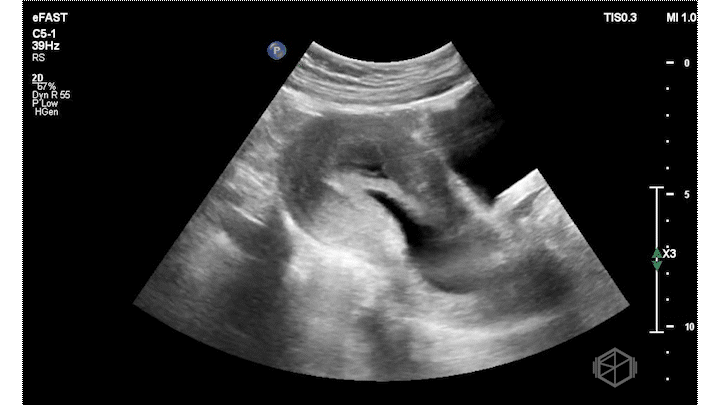
On this presentation Dr. Salman saw the following:
The ultrasound above shows an irregular appearing gestational sac with an irregular appearing structure intra-gestational sac without evidence of a heartbeat. Given this patient already had an US suggestive of pregnancy failure and she had heavy bleeding, this is indicative of pregnancy failure and inevitable vs. less likely incomplete abortion. She was taken to the OR for a D&C and discharged after the procedure without complications.
Diagnosis: Pregnancy failure with inevitable vs. incomplete abortion
Learning points:
A pregnant patient with a positive HCG but no visible gestational sac or ectopic pregnancy on transabdominal or preferably transvaginal ultrasound is labeled as having a pregnancy of unknown location.
This should be correlated with HCG levels, clinical examination, and the patient's pregnancy intentions. A stable patient may follow the ectopic precaution protocol and return in 48 hours for repeat HCG and possible ultrasound.
A patient with a gestational sac should be evaluated for the presence of a definite intrauterine pregnancy (the presence of a yolk sac, the first definitive sign of an IUP).
Transvaginal US is used to determine the viability and there are specific criteria necessary for pregnancy failure (24106937). See table below based on the NEJM article:
| Guidelines for Transvaginal Ultrasound Diagnosis of Pregnancy Failure in a Patient with IUP of uncertain viability | |
|---|---|
| Findings diagnostic of pregnancy failure | CRL ≥ 7mm, no HR MSD ≥ 25mmg, no embryo No embryo with HR ≥ 2 weeks after scan that showed GS without YS No embryo with HR ≥ 11 days after scan that showed GS with YS |
| Findings suspicious for, but not diagnostic of, pregnancy failure | CRL < 7mm, no HR MSD 16-24mm, no embryo No embryo with HR 7-13 days after scan that showed GS without YS No embryo with HR 7-10 days after scan that showed GS with YS Absence of embryo ≥ 6 weeks after LMP Empty amnion (seen adjacent to YS, no visible embryo) Enlarged YS (>7mm) Small GS in relation to size of embryo (<5mm difference between MSD and CRL) |
A patient with heavy vaginal bleeding and IUP of uncertain viability or findings diagnostic of pregnancy failure should be considered a potentially unstable incomplete or inevitable abortion and Ob/Gyn should be immediately consulted (39406415).